Med info
Early-stage cataracts: When to monitor and when to intervene? A guide to early medical decision-making
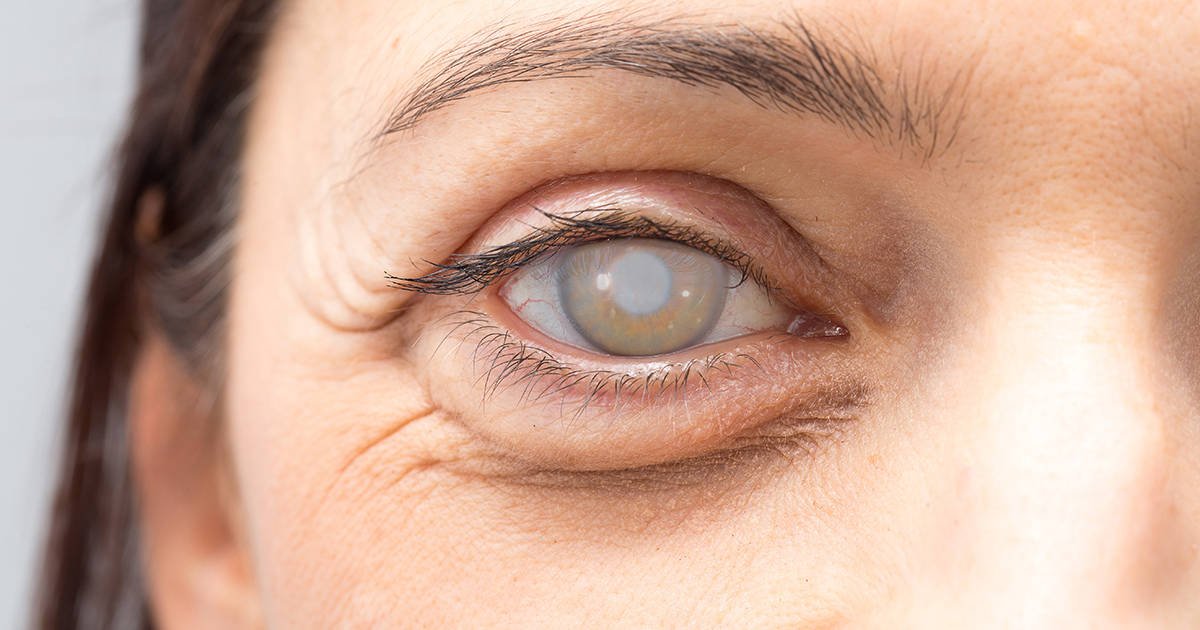
What is meant by early-stage cataract?
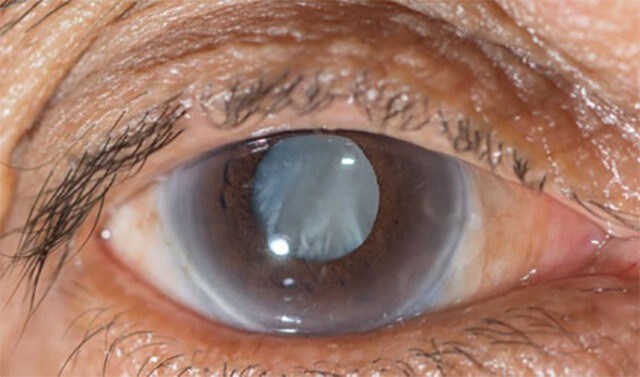
Early-stage cataract refers to the initial formation of mild clouding in the eye’s normally clear crystalline lens. At this point, the opacity begins to affect visual clarity gradually, but symptoms are usually not severe or significantly disruptive to daily activities.
In this early phase, a person may notice slightly blurred vision, mild difficulty seeing at night, increased sensitivity to glare or halos around lights—especially while driving at night—or a need to change their eyeglass prescription more frequently.
Early cataracts typically progress slowly with aging, but they can also be associated with diabetes, long-term use of corticosteroids, or chronic exposure to sunlight without adequate eye protection.
Diagnosis of early-stage cataract is made through a comprehensive eye examination by an ophthalmologist, using a slit-lamp biomicroscope to evaluate the lens. This helps monitor the progression of the cataract and determine the appropriate timing for surgical intervention, if and when it becomes necessary.
Understanding what an early cataract is can be reassuring for patients, since this stage usually does not require immediate surgery. Instead, it calls for regular follow‑up and adopting a healthy lifestyle to help preserve vision for as long as possible.
How do cataracts start? (What happens inside the eye)
Gradual Loss of Lens Transparency
In the early stages of cataract formation, vision doesn’t deteriorate suddenly. Instead, the normally clear crystalline lens of the eye gradually starts to lose its transparency.
Over time, the structure of the lens changes and its ability to transmit light sharply to the retina declines. The person may begin to notice slightly blurred or washed‑out vision, especially when looking at distant objects or in bright light.
This subtle reduction in lens clarity is the first step in cataract development. It often goes unnoticed in the early stages because it is limited to a small area of the lens and doesn’t significantly affect overall vision at first.
Protein Buildup Inside the Lens
The eye’s lens contains proteins arranged in a very precise way to keep it clear and transparent.
When a cataract starts to form, these proteins begin to clump together instead of remaining evenly distributed, creating tiny cloudy areas within the lens.
These protein aggregates interfere with the smooth passage of light, causing the patient to experience a slight haze in front of the eye or mild visual blurring, particularly when reading or driving at night.
This buildup of proteins inside the lens is the main mechanism that explains what happens within the eye during the early stages of cataract development.
The Role of Age and Health Factors
Cataracts most commonly develop with advancing age due to natural changes in the lens tissue, which gradually becomes harder and less transparent over the years.
Certain health conditions—such as diabetes, high blood pressure, long‑term use of corticosteroids, and chronic exposure to ultraviolet (UV) sunlight—also accelerate these changes in the eye.
These factors increase damage to the lens fibers and proteins, speeding up the onset of cataracts and causing symptoms to appear earlier or more noticeably.
Understanding the influence of age and overall health helps explain why cataracts start earlier in some people and why they progress more rapidly in certain cases than in others.
Why Cataracts Usually Progress Slowly
In most people, cataracts progress slowly because the changes inside the lens occur very gradually.
The process of protein accumulation and loss of transparency does not take place over days or weeks; it typically unfolds over several years. As a result, the brain gradually adapts to the declining image quality, and the patient may not notice a problem until the visual impairment becomes more pronounced.
In addition, the cloudy areas usually begin in a small part of the lens and do not initially block a large amount of light, so vision can remain relatively satisfactory for quite some time.
This slow progression explains why an ophthalmologist may detect cataracts during a routine eye examination before the patient is aware of any obvious changes in vision.
Early Cataract Symptoms – Should You Be Worried?

Mild blurred vision (especially in low light)
In the early stages of cataract, patients may notice mild blurring of vision, which becomes more obvious in dimly lit environments or when trying to read at night.
This blurring is often intermittent at first, and some people may attribute it to eye strain or needing a stronger glasses prescription, while in reality it can be one of the earliest signs of developing cataracts.
As the clouding of the crystalline lens progresses, night vision becomes more hazy, and the person starts to struggle with seeing fine details, especially when looking at distant objects or in relatively dark places.
Therefore, if you notice recurrent episodes of blurred vision in low light, it is important not to ignore this sign and to see an ophthalmologist to determine whether it is related to early-stage cataract or another cause.
Increased light sensitivity (photophobia)
One of the common early symptoms of cataract is increased sensitivity to light, especially bright sunlight or intense white artificial lighting.
The affected person may feel discomfort or a mild aching sensation in the eyes when exposed to direct light sources, or feel the need to close the eyes or wear sunglasses more frequently than usual.
This sensitivity occurs because the clouded lens no longer handles light normally; instead, light is scattered inside the eye, causing an uncomfortable sensation in bright conditions.
If you notice that your eyes have become more sensitive to light than before, particularly along with mild blurred vision, this may be an early indicator of cataract and warrants a thorough eye examination.
Seeing halos around lights
Seeing halos or glowing rings around light sources, such as car headlights or street lamps, is another early sign that may indicate the presence of cataract.
These halos usually appear more clearly at night or in dark environments when there is a strong light source, making the person see the light as if surrounded by one or more diffuse luminous circles.
This phenomenon occurs because light is scattered within the opacified lens and no longer focuses accurately on the retina, which distorts the appearance of light sources in the visual field.
Halos around lights can resemble symptoms of other eye conditions such as glaucoma, so self‑diagnosis is unreliable; a proper evaluation by an ophthalmologist is essential to determine the exact cause.
Difficulty driving at night
Difficulty driving at night is one of the most noticeable symptoms in the early stages of cataract, particularly when facing oncoming headlights.
The patient feels that vision is less clear in the dark, with bothersome glare from car headlights or streetlights, which reduces confidence while driving and may even lead to avoiding night driving altogether.
Several early cataract symptoms overlap in this situation, such as blurred vision, halos, and increased light sensitivity, making it harder to recognize roads, pedestrians, and traffic signs.
If you begin to feel that driving at night has become more difficult or less safe than before, this may be related to early cataract, and an early eye check‑up is recommended to prevent complications that could compromise driving safety.
Frequent changes in glasses prescription
Needing to change your eyeglasses frequently—whether in terms of prescription strength or clarity of vision—can be an early sign of cataract.
Some people notice that the glasses that were adequate only a few months ago no longer provide the same visual sharpness, leading them to change lenses repeatedly without satisfactory improvement.
This happens because the crystalline lens itself gradually changes and becomes more opaque, altering how light is refracted inside the eye and causing unstable visual acuity.
If you find yourself needing to adjust your glasses or contact lens prescription more often than usual, especially if you also have blurred vision or difficulty seeing at night, it is important to consider the possibility of cataract and undergo a comprehensive eye examination by an ophthalmologist.
When Is Observation Alone Enough?

When vision is still adequate for daily life
In the early stages of cataract, simple observation may be sufficient if vision is still good enough to carry out normal daily activities such as reading, using a smartphone, and watching television.
At this stage, lens opacity is usually mild and does not significantly affect quality of life, so ophthalmologists often prefer regular follow‑up rather than rushing into cataract surgery.
The main goal is to monitor the progression of the cataract, and to see an eye specialist promptly if there is any noticeable decline in visual acuity or an increase in blurriness.
When there is no impact on work or driving
Observation alone is often appropriate when an early cataract does not impair a person’s ability to work or drive safely.
If the patient can perform work accurately—especially tasks that require clear vision, such as computer work or operating machinery—and has no difficulty driving during the day or at night, periodic follow‑up is usually sufficient at this stage.
Here, the ophthalmologist focuses on assessing how the cataract affects personal safety. If there is no risk to the patient or others while driving or working, cataract surgery can be postponed and regular eye examinations maintained.
When symptoms are not progressing rapidly
One of the key situations in which watchful waiting is appropriate is when cataract symptoms are not worsening quickly.
If symptoms remain stable for a long period—for example, mild blurred vision or slight light sensitivity without obvious deterioration—the doctor may recommend follow‑up every 6–12 months to monitor cataract progression.
Regular monitoring helps detect any acceleration in lens opacity early, while sparing the patient from cataract surgery as long as symptoms remain stable and do not significantly interfere with daily life.
When vision can be improved with glasses
If vision can be improved with a new eyeglass prescription or by adjusting the current one, many ophthalmologists prefer to rely on observation alone in the early stages of cataract.
At this point, lens clouding is usually mild and can be partially compensated for with refractive correction, which may delay the need for cataract surgery.
It is important for the patient to wear the appropriate glasses consistently and to revisit the eye doctor if they no longer provide the same clarity, as this may indicate that the cataract is progressing.
Situations in which doctors prefer follow‑up only
Ophthalmologists often choose simple follow‑up in several scenarios, such as early‑stage cataracts with minimal symptoms, or in elderly patients who do not experience visual difficulty and are not interested in surgery at the moment.
They may also recommend observation if there are other eye conditions or systemic diseases that make the timing of surgery less suitable, in which case cataract surgery is postponed until it can be performed more safely.
In all these situations, regular check‑ups and comprehensive eye examinations are essential, with continuous assessment of visual acuity and the impact of cataract on daily functioning before making a final decision about surgery.
How is cataract monitored without intervention?
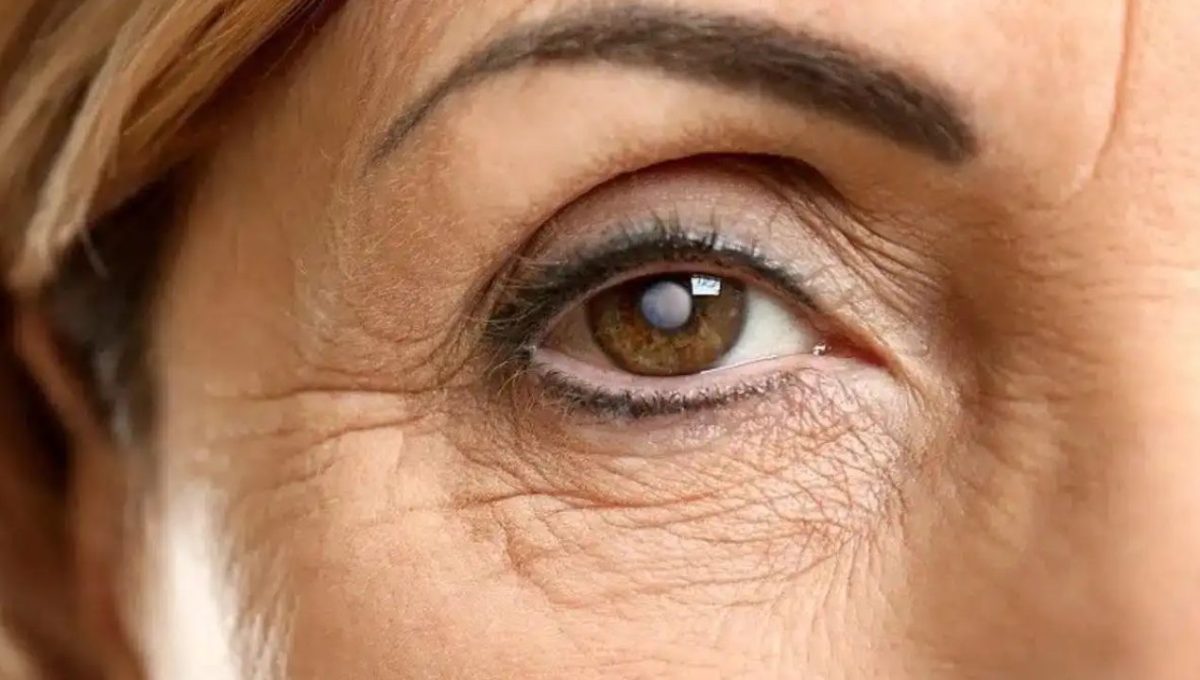
Frequency of follow‑up (typically every 6–12 months)
In the early stages of cataract, the condition is usually monitored without surgery through regular follow‑up visits to the ophthalmologist, typically every 6–12 months. The exact interval depends on how rapidly the lens opacities are progressing and on the patient’s visual status.
This schedule is designed to track early cataract progression and ensure the patient can still see well enough to carry out daily activities without needing surgery.
In certain cases—such as patients with diabetes or coexisting eye diseases—the doctor may recommend more frequent visits to closely monitor the condition and prevent deterioration.
Organizing follow‑up in this way helps determine the right time for intervention and allows safe monitoring without immediate surgery.
Key assessments (visual acuity – lens examination)
During conservative follow‑up of early‑stage cataracts, the ophthalmologist relies on several core examinations, most importantly visual acuity testing and lens evaluation.
Visual acuity is measured using an eye chart to assess distance and near vision and to document any gradual decline in the ability to read or see fine details.
The lens is examined with a slit‑lamp biomicroscope to assess the degree and location of lens opacity and its actual impact on the passage of light through the eye.
Additional tests such as intraocular pressure measurement and dilated fundus examination may be performed to rule out other ocular conditions that could influence the decision to continue observation without intervention.
These periodic assessments give the physician a clear picture of cataract progression and support an informed decision about the optimal timing of surgery when indicated.
Monitoring changes in symptoms
As part of non‑surgical cataract follow‑up, special attention is paid to how the patient’s symptoms evolve over time.
Key symptoms to monitor include: blurred vision, difficulty seeing at night, increased sensitivity or glare from lights, frequent changes in eyeglass prescription, and problems with reading or driving.
At each visit, the doctor compares the patient’s current complaints with those recorded previously to determine whether the early cataract is stable or whether symptoms are starting to affect quality of life.
If symptoms are mild and do not interfere with daily activities, follow‑up without surgery can continue, possibly with adjustments such as better lighting or updating spectacles.
However, if there is ongoing deterioration in symptoms, this becomes a signal to reconsider simple observation and start discussing surgical options.
The patient’s role in noticing changes
Successful monitoring of early‑stage cataracts without surgery depends heavily on the patient’s awareness and active participation in noticing any visual changes.
Patients are advised to pay attention to new difficulties with reading, increased glare from sunlight or headlights at night, colors appearing duller, or double vision in one eye.
It is important to record these changes and report them to the ophthalmologist at the next visit—or book an earlier appointment if the symptoms are bothersome or appear suddenly.
Patients are also encouraged to periodically test each eye separately to detect any significant difference that might indicate faster progression in one eye.
This active role helps ensure accurate follow‑up and timely detection of the point at which management should shift from comfortable observation to intervention.
When to move from “observation” to “intervention”
During conservative management of early cataracts, the decision to move from “observation” to “intervention” is made when the cataract starts to clearly interfere with the patient’s lifestyle.
Surgery is considered when visual acuity declines to the point that everyday tasks—such as reading, working, or driving—are impaired, or when normal lighting becomes insufficient and glare from lights is significantly increased.
Transition from observation to intervention is also recommended if cataract‑related complications develop, or if satisfactory vision can no longer be achieved with glasses or contact lenses.
The decision is not based solely on visual acuity numbers but on a comprehensive evaluation that integrates clinical findings, the patient’s symptoms, and overall quality of life.
Once the cataract reaches this stage, surgery becomes the best option to restore clearer vision rather than continuing with observation alone.
When Does Intervention Become Necessary?
Noticeable decline in visual quality
Intervention for early-stage cataracts becomes necessary once you begin to experience a clear and bothersome deterioration in visual quality that affects your daily activities.
If you start seeing objects as hazy or blurred, notice that colors look washed out, or find it difficult to distinguish fine details even in good lighting, this may indicate that the cataract has progressed beyond a mild stage and now requires a thorough evaluation by an ophthalmologist.
At this point, simply changing your glasses is no longer sufficient. Medical—and possibly surgical—intervention is considered if the opacity of the crystalline lens is preventing you from carrying out your usual activities comfortably.
Difficulty reading or working
When early cataracts cause persistent difficulty with reading, office work, or using a computer—despite good lighting and appropriate prescription glasses—this is a sign that the time for intervention is approaching.
If you find yourself needing to enlarge text excessively, reading very slowly, or experiencing rapid eye strain while working, the persistence of these symptoms suggests that the impact of the cataract has gone beyond a minor inconvenience and has started to reduce your productivity and professional quality of life.
In such cases, it is advisable to consult an ophthalmologist to review treatment options and determine whether continued monitoring is sufficient or whether you should begin planning for cataract surgery.
Driving problems, especially at night
One of the most significant warning signs that intervention is becoming necessary is the appearance of clear difficulties while driving, particularly at night.
If you begin to notice increased glare from oncoming headlights, halos around light sources, or trouble seeing the road and traffic signs in the dark, this indicates that the lens of the eye has become more opaque.
These changes do not only affect comfort while driving; they also increase the risk of accidents.
When cataracts reach this stage, ophthalmologists often recommend seriously considering treatment before driving becomes completely unsafe.
Vision not improving with glasses
In the early phases of cataract development, vision may improve temporarily by changing the eyeglass prescription. However, if you find that changing your glasses multiple times no longer provides clear vision, this is a strong indication that intervention is becoming necessary.
When vision no longer improves with new glasses, it means the problem is not just a refractive error, but a loss of transparency in the lens itself.
At this stage, your ophthalmologist will begin discussing cataract extraction as an effective way to restore visual clarity, rather than repeatedly adjusting your prescription with no real benefit.
Impact on lifestyle
The decisive factor in determining when intervention is necessary in early-stage cataracts is how much the condition is affecting your lifestyle.
If you start avoiding going out at night, cutting back on reading, hesitating to travel or drive long distances, or feeling that poor vision is limiting your independence and self-confidence, then the cataract is no longer a mild condition that can simply be observed.
Once cataracts begin to interfere with your hobbies, work, and social life, medical—and often surgical—treatment becomes the appropriate option to safely restore your visual clarity and overall quality of life.
What happens if cataract treatment is delayed?
Putting off cataract treatment in its early stages can gradually lead to a marked decline in visual quality and increasing difficulty with everyday activities such as driving, reading, and using digital screens. This in turn raises the risk of accidents and loss of independence.
As the cataract becomes denser, vision turns progressively more blurred and yellowish. You may start noticing halos around lights and a significant reduction in night vision, which can cause ongoing eye strain and frequent headaches.
In advanced, neglected cases, cataracts can lead to severe visual impairment, to the point where even recognizing faces or detecting movement in front of you becomes challenging. At this stage, surgery may be more complex and the lens harder to remove, sometimes requiring additional surgical steps.
Leaving cataracts untreated for a long time can also increase the risk of elevated intraocular pressure and secondary glaucoma, as well as other retinal complications, all of which threaten long‑term eye health.
For these reasons, it is strongly recommended to consult an ophthalmologist as soon as early symptoms of cataract appear. Timely intervention allows vision to be restored safely and helps prevent progression to advanced complications.
Best Cataract Specialist in Jeddah
Dr. Issa Baessa: Subspecialized Expertise in Cataract Surgery and Intraocular Lens Implantation
Dr. Issa Baessa is widely regarded as one of the leading cataract surgeons in Jeddah, particularly for patients in the early stages of cataract who require precise evaluation and an individualized treatment plan.
Dr. Baessa has extensive experience in early cataract diagnosis using state-of-the-art imaging and diagnostic devices for the lens and retina. This enables him to establish an appropriate follow‑up strategy or recommend timely surgical intervention before symptoms progress and significantly impair visual quality.
In the field of cataract (lens opacity) surgery, Dr. Issa Baessa utilizes advanced techniques such as phacoemulsification through micro‑incisions, combined with the implantation of high‑precision intraocular lenses (IOLs). This approach helps enhance visual clarity and reduce dependence on glasses as much as possible.
His meticulous approach to selecting the most suitable lens for each patient—whether monofocal, multifocal, or toric lenses for the correction of astigmatism—makes him a preferred choice for those seeking the best cataract specialist in Jeddah and aiming for stable, comfortable long‑term visual outcomes.
By combining refined surgical skills with cutting‑edge technology, Dr. Issa Baessa provides comprehensive care for patients with early‑stage cataract, from initial screening and diagnosis through to cataract extraction and lens implantation, ensuring the highest standards of safety and visual quality for patients in Jeddah.
Book Your Cataract Screening Now at Batal Eye Specialty Center – Start Your Journey to Clearer Vision with Top Eye Doctors in Jeddah
When cataracts are detected in their early stages, they are much easier to manage and the need for more advanced surgical intervention can often be reduced. That’s why scheduling regular eye examinations is essential for preserving the quality of your vision.
At Batal Eye Specialty Center in Jeddah, our team of leading ophthalmologists provides comprehensive eye screenings using state-of-the-art diagnostic technology to:
- Detect cataracts in their earliest stages
- Assess how much they are affecting your vision
- Design a personalized treatment plan tailored to your condition and lifestyle
Early examination helps you recognize cataract symptoms such as blurred or cloudy vision, poor night vision, and increased sensitivity to light, so you can make the right medical decision at the right time—before the problem progresses.
Book your eye exam today at Batal Eye Specialty Center in Jeddah and begin your journey toward clearer vision, with specialized medical care and advanced treatment options designed to protect you from the long-term complications of cataracts.





