Med info
Who Is Not a Candidate for Laser Vision Correction? Complete Guide to Contraindications
Conditions That Permanently Contraindicate Laser Vision Correction
Certain medical conditions constitute absolute contraindications to laser vision correction, even with current advanced technologies.
Most notably, markedly thinned corneas or severe corneal ectasias such as keratoconus make procedures like LASIK unsafe, as surgical intervention can further weaken the cornea and lead to irreversible visual deterioration.
Uncontrolled autoimmune disorders, including systemic lupus erythematosus and rheumatoid arthritis, are also considered major contraindications, as they impair corneal healing and significantly increase the risk of postoperative complications.
In addition, procedures such as LASIK and femto-LASIK are avoided in the presence of active or chronic ocular surface inflammation, advanced retinal disease, or markedly elevated and uncontrolled intraocular pressure (glaucoma), as surgery in these situations may worsen pre-existing visual damage.
Patients are likewise excluded from refractive surgery if they have advanced retinitis pigmentosa or severe corneal thinning resulting from previous corneal surgeries.
In such cases, ophthalmologists typically recommend relying on eyeglasses, contact lenses, or other safer alternatives, rather than exposing the eye to the risks associated with laser vision correction.

Keratoconus and Other Corneal Ectatic Disorders
Keratoconus is one of the main conditions that absolutely contraindicate laser vision correction, as it leads to a marked loss of corneal rigidity and biomechanical stability.
In keratoconus, the cornea becomes thin and irregularly shaped, which makes laser procedures such as LASIK, Femto‑LASIK, or even surface ablation (PRK) unsafe.
Performing laser on a cornea affected by keratoconus can accelerate progression of the disease, increase corneal protrusion, and worsen visual distortion.
Therefore, once keratoconus or any corneal ectatic disorder is diagnosed through corneal topography and pachymetry, refractive surgeons will decline to perform laser vision correction in order to protect the eye.
In such situations, other options are considered instead of laser, such as corneal collagen cross‑linking, rigid gas‑permeable lenses, or intrastromal corneal ring segments (ICRS).
Inadequate Corneal Thickness for Laser Procedures
Corneal thickness is a critical parameter in deciding whether laser vision correction can be safely performed.
If the cornea is not thick enough, removing tissue with an excimer laser becomes dangerous, as it may compromise corneal integrity and result in serious complications such as post‑LASIK ectasia.
For this reason, having a corneal thickness below the minimum safe threshold is considered a definitive contraindication to laser vision correction in many patients.
Corneal thickness is measured using advanced devices such as the Pentacam or pachymetry. If these tests show a very thin cornea, the ophthalmologist will advise against any laser procedure on the corneal surface.
Alternative options may then be suggested, such as prescription contact lenses or phakic intraocular lenses (IOLs), instead of corneal laser surgery.

Advanced Retinal Disease or Previous Retinal Detachment
Advanced retinal diseases—such as severe diabetic retinopathy, advanced age‑related macular degeneration, or a history of retinal detachment—are major reasons to permanently rule out laser vision correction.
Visual acuity depends primarily on the health of the retina, especially the macula, even if the cornea and crystalline lens are normal.
When the retina is significantly damaged, laser vision correction will not meaningfully improve sight and may expose the eye to additional risks without real benefit.
Moreover, in cases of previous retinal detachment or a high predisposition to new detachment, changes in intraocular pressure during or after surgery may increase the risk of further retinal deterioration.
Therefore, a thorough dilated fundus examination is always performed before considering any refractive surgery. If advanced retinal pathology is present, it is regarded as a permanent contraindication to laser vision correction.
Uncontrolled or Unstable Glaucoma
Glaucoma (ocular hypertension with optic nerve damage) is a chronic disease that affects the optic nerve, usually due to elevated intraocular pressure.
When glaucoma is uncontrolled or unstable despite medications or prior surgery, laser vision correction is considered unsafe.
After LASIK and similar procedures, intraocular pressure readings can be falsely low because of reduced corneal thickness, complicating accurate glaucoma monitoring and management.
In addition, intraoperative and postoperative fluctuations in intraocular pressure may further compromise an already vulnerable optic nerve.
For these reasons, uncontrolled glaucoma is regarded as a contraindication to laser vision correction, and physicians prioritize stabilizing intraocular pressure and preserving the optic nerve over any refractive procedure.
Visually Significant Cataract
When cataract (lens opacity) progresses to the point that it significantly impairs visual clarity, performing corneal laser vision correction is no longer reasonable.
In such cases, the primary issue is not corneal refractive error but opacification of the intraocular lens, which LASIK, Femto‑LASIK, or PRK cannot address.
Thus, a visually significant cataract is a definitive contraindication to corneal laser surgery, and the patient is advised to undergo cataract extraction with intraocular lens implantation.
By replacing the cloudy lens with a clear intraocular lens of appropriate power, most refractive errors—such as myopia, hyperopia, and astigmatism—can be corrected without resorting to laser on the cornea.
Accordingly, any patient with reduced vision due to advanced cataract is directed first to cataract surgery rather than laser vision correction.
Medical conditions that may rule out laser vision correction
There are several medical conditions that can make a patient unsuitable for laser vision correction, or require postponing the procedure until the condition is stable.
Key contraindications include autoimmune diseases such as systemic lupus erythematosus (SLE) and rheumatoid arthritis, as well as conditions that impair wound healing such as poorly controlled diabetes, as these can increase the risk of corneal complications and delay recovery.
Chronic eye diseases are also a major reason to avoid the surgery, particularly keratoconus, severe dry eye disease, previous corneal injuries, or significant corneal thinning. In such cases, the corneal surface is not robust enough to tolerate safe removal of corneal tissue.
Patients may also be considered unsuitable if they have severe immune system disorders, or if they are taking medications that suppress immunity or cause marked ocular dryness, such as some systemic acne treatments (e.g., isotretinoin).
The ophthalmologist will review the patient’s full medical history, including uncontrolled hypertension, bleeding disorders, and whether the patient is pregnant or breastfeeding, to ensure that laser vision correction can be performed safely and that the outcome will remain stable in the long term.
Autoimmune Diseases (Lupus, Rheumatoid Arthritis, Psoriasis, etc.)
Autoimmune conditions such as systemic lupus erythematosus, rheumatoid arthritis, and psoriasis are among the most important factors that can make a patient unsuitable for laser vision correction.
In these disorders, the immune system attacks the body’s own healthy tissues, including the cornea and conjunctiva. This can compromise corneal healing after surgery and significantly increase the risk of complications such as infections, severe dry eye, or deterioration in visual acuity.
For this reason, ophthalmologists usually advise against vision correction procedures in patients with poorly controlled autoimmune disease, or recommend postponing surgery until the condition is adequately stabilized under the care of a rheumatologist or immunology specialist.
A thorough medical assessment and close coordination between the ophthalmologist and the treating specialist are essential before considering any form of refractive surgery, such as LASIK or femto-LASIK.
Uncontrolled Diabetes with Diabetic Retinopathy
Patients with poorly controlled diabetes, especially those with diabetic retinopathy, are often considered poor candidates for laser vision correction.
Fluctuating and elevated blood glucose levels can alter corneal thickness and the crystalline lens, leading to unstable refraction and variable prescriptions — and stable measurements are a fundamental requirement before any refractive procedure.
Moreover, diabetes impairs the microcirculation of the eye and can negatively affect corneal wound healing, while increasing the likelihood of infection or delayed recovery after LASIK or surface ablation procedures (such as PRK).
When diabetic retinopathy is present, the primary goal becomes treating the retina and preserving remaining vision rather than eliminating the need for glasses. In such cases, surgeons commonly recommend avoiding refractive surgery until diabetes is well controlled and the ocular condition has stabilized.
Medications that Affect Corneal Healing (Corticosteroids, Isotretinoin/Accutane)
Certain medications may temporarily render a patient unsuitable for laser vision correction because they directly interfere with corneal healing and the integrity of the ocular surface.
Long-term use of corticosteroids can suppress local immune defenses in the eye, increase the risk of infection, and delay tissue repair following surgery.
Anti-acne medications such as isotretinoin (Accutane) are well known for causing significant ocular dryness and destabilizing the tear film, which increases the risk of corneal epithelial breakdown and post-LASIK complications.
Therefore, refractive surgeons typically require discontinuation of these drugs for a specified period before considering any laser procedure, along with a detailed evaluation of corneal health, tear film stability, and overall readiness of the eye for surgery.
History of Chronic Dry Eye
Chronic dry eye is one of the most important conditions that can make a patient a questionable or poor candidate for laser vision correction, or at least warrant extreme caution before proceeding.
Most laser vision correction procedures depend on a healthy corneal surface and a stable tear film, as any disturbance in ocular lubrication can directly affect both visual quality and corneal healing.
Patients with chronic dry eye often experience burning, foreign body sensation, and persistent redness. These symptoms can become markedly worse after surgery and may lead to blurred vision and difficulty performing routine daily activities.
For this reason, the ophthalmologist will carefully assess and treat dry eye disease before surgery, often intensifying therapy. If the dryness is severe or remains unstable, the physician may recommend postponing or avoiding refractive surgery altogether to protect the patient’s ocular health and ensure reliable visual outcomes.
Temporary Conditions That Can Prevent Laser Vision Correction
There are several temporary medical conditions that may prevent an ophthalmologist from safely performing laser vision correction, even if the patient is otherwise suitable in terms of age and degree of refractive error.
The most important of these include active eye infections such as conjunctivitis or keratitis, and uncontrolled severe dry eye, as these problems can increase the risk of complications and interfere with proper corneal healing after surgery.
It is also recommended to postpone laser vision correction during pregnancy and breastfeeding due to hormonal changes that can temporarily affect the refractive error and corneal response, which may in turn impact the accuracy and stability of the surgical outcome.
In addition, contact lenses must be discontinued for a period determined by the doctor before preoperative measurements, as lenses can temporarily alter the corneal shape and lead to inaccurate readings.
In all of these situations, the contraindication is temporary. The patient’s eligibility for laser vision correction can be reassessed once the underlying issue has been treated and the refraction has stabilized, in order to achieve the best possible results with maximum safety.
Pregnancy, Breastfeeding, and the Impact of Hormones on Vision Correction Measurements
During pregnancy and breastfeeding, hormone levels in the body fluctuate significantly, which can temporarily affect the cornea and refractive error.
Women may notice changes in visual acuity, increased dry eye, or blurred vision. These symptoms often resolve once pregnancy is over or breastfeeding has stopped.
For this reason, refractive surgeons advise postponing any laser vision correction procedure (such as LASIK or PRK) until hormones have stabilized and refraction has returned to baseline—usually about 3–6 months after the end of breastfeeding.
Undergoing vision correction during this period can lead to inaccurate outcomes or the need for enhancement procedures later on.
Therefore, pregnancy and breastfeeding are considered temporary contraindications to refractive surgery, in order to protect patient safety and ensure the best possible long‑term results.
Active Eye Infections or Severe Allergic Eye Disease
The presence of active ocular infections—such as bacterial or viral conjunctivitis—or severe, chronic ocular allergy is among the most important temporary contraindications to laser vision correction.
An inflamed or irritated cornea is more prone to complications, including delayed epithelial healing, worsening dryness, or even deterioration in visual quality after surgery.
In addition, frequent eye rubbing due to allergy and itching can exert mechanical pressure on the cornea after LASIK, potentially compromising the stability of the surgical result.
Accordingly, eye infections must first be fully treated, and allergic eye disease brought under control with anti-allergic eye drops and lubricating artificial tears. Only after complete resolution should the eyes be reassessed before considering any refractive procedure.
This approach maximizes safety and improves the chances of long-term success for laser vision correction.
Unstable Refraction During the Previous Year
A fundamental requirement for successful refractive surgery is stable refraction for at least 12 months.
If there has been a notable change in prescription over the past year—whether an increase or decrease in myopia, hyperopia, or astigmatism—this is considered a temporary barrier to proceeding with surgery.
Refractive instability indicates that the eye is still undergoing change, especially in younger patients or those with rapidly progressing myopia. In such cases, LASIK or femto-LASIK may not provide the lasting correction the patient expects.
If surgery is performed while the refraction is still changing, the patient may later require enhancement surgery or may still need to wear glasses.
Therefore, ophthalmologists usually recommend postponing the procedure and monitoring refraction regularly until it stabilizes, then re‑evaluating candidacy to ensure the most predictable and durable outcome.
Long-Term Contact Lens Wear Before Evaluation Without Allowing the Cornea to Recover
Contact lenses—especially rigid (RGP) lenses, but also soft lenses worn for many hours a day—can temporarily alter the shape of the cornea.
These shape changes can affect the accuracy of refraction and corneal topography, both of which are crucial for planning laser vision correction.
If the eyes are not given sufficient time out of contact lenses before preoperative testing, the measurements obtained may be misleading, resulting in an inappropriate laser treatment plan and suboptimal visual outcomes.
For this reason, ophthalmologists advise discontinuing soft contact lenses for at least 3–7 days before evaluation, and stopping rigid lenses for up to two weeks or longer, depending on the individual case.
During this “contact lens holiday,” the cornea returns to its natural contour, allowing for reliable refractive measurements and an accurate assessment of candidacy for safe and effective vision correction surgery.
Anatomical Eye Problems That Can Contraindicate Surgery
One of the most important reasons to avoid vision correction surgery is the presence of anatomical problems in the eye that make laser procedures unsafe or ineffective.
In some patients, the cornea may be too thin or irregularly shaped, as in keratoconus or in early corneal thinning disorders. This significantly raises the risk of serious complications, such as corneal ectasia (progressive corneal bulging) or deterioration in visual quality after surgery.
Certain corneal abnormalities—like marked irregularity, deep corneal scars, or a history of previous eye surgery—can also rule out procedures such as LASIK and Femto-LASIK.
In addition, a very large pupil size in low light, abnormally small palpebral aperture, or deformities of the eyelids or ocular surface (such as severe dry eye or chronic inflammatory conditions) can make the visual outcome of refractive surgery unpredictable.
For these reasons, ophthalmologists perform detailed preoperative assessments, including corneal pachymetry (measuring corneal thickness), corneal topography (mapping the corneal surface), and a thorough fundus examination to ensure there are no anatomical issues that would contraindicate or limit laser vision correction.
Irregular Corneal Curvature (Irregular Astigmatism)
An abnormal curvature of the corneal surface, known as irregular astigmatism, is considered one of the most significant anatomical issues of the eye that may lead to ineligibility for laser vision correction.
In this condition, the corneal surface is uneven, which distorts the way light passes into the eye and makes it difficult to obtain an accurate measurement of the refractive error.
This type of astigmatism is often not fully correctable with standard glasses or conventional contact lenses, making its management with LASIK or Femto-LASIK more complex.
In cases of marked irregular astigmatism, the surgeon may consider it a contraindication to laser vision correction, since these procedures depend on reshaping the corneal surface with extreme precision. Any significant irregularity can increase the risk of visual disturbances such as blurred vision, glare, or halos and compromise visual quality after surgery.
For this reason, detailed corneal assessments such as corneal topography are performed before deciding on any refractive procedure, to confirm that the corneal surface is regular and suitable for surgical intervention.
Excessive Pupil Dilation in Low Light
Excessive pupil dilation in dim lighting is another anatomical factor that may make the surgeon hesitant to proceed with laser vision correction.
When the pupil becomes very large in low-light conditions, light enters through the peripheral zones of the cornea, where the laser effect is less precise, which may lead to bothersome postoperative visual symptoms.
These symptoms include halos around lights, night glare, and reduced vision in the dark—complaints that significantly affect quality of life, especially for those who drive at night or work in low‑light environments.
Therefore, measuring pupil size in both light and dark conditions is an essential part of the preoperative assessment for refractive surgery. Marked pupil dilation may be considered a relative contraindication to the procedure, or it may require choosing a specific laser technique designed to reduce these risks.
Understanding this point helps patients realize that, in some cases, the decision to decline surgery is actually made to protect them from long‑term visual problems after the operation.
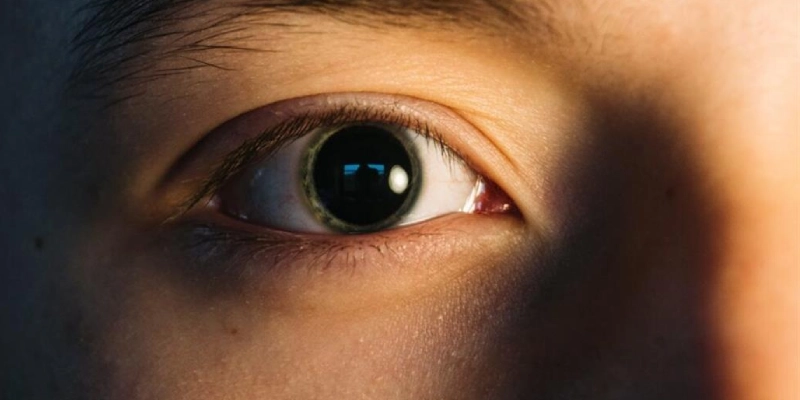
Corneal Thickness Below the Safe Limit for LASIK
Corneal thickness is one of the most critical anatomical parameters evaluated before performing any type of laser refractive surgery, such as LASIK or Femto‑LASIK.
If the cornea is thinner than the established safety threshold, this is considered a contraindication to laser vision correction, because the procedure works by removing part of the corneal tissue to reshape it and correct myopia, hyperopia, or astigmatism.
In a thin cornea, removing too much tissue can weaken its structural integrity and increase the risk of serious complications such as corneal ectasia (post‑LASIK keratoectasia) or long‑term visual distortions.
For this reason, ophthalmologists insist on performing corneal thickness measurement (pachymetry) as a fundamental step before any laser procedure. If the cornea is found to be too thin, the surgery is either declined or an alternative is recommended, such as implantable intraocular lenses instead of reshaping the cornea.
In this way, insufficient corneal thickness becomes one of the main anatomical reasons to avoid laser vision correction, in order to preserve ocular safety and maintain good visual quality over the long term.
Tests That Show You’re Not a Good Candidate for Vision Correction Surgery
Before deciding on laser vision correction, an ophthalmologist performs a series of detailed examinations to determine whether your eyes are suitable for this type of procedure.
These tests may show that a patient is not a good candidate if the cornea is thinner than the safe threshold, or if it has a conical or irregular shape, as seen in conditions like keratoconus.
Corneal mapping and corneal topography can also reveal surface irregularities that may increase the risk of complications after LASIK or femto-LASIK.
In addition, tests such as intraocular pressure measurement, dilated fundus examination, and assessment of the degree of myopia, hyperopia, or astigmatism may uncover unstable refractive error or eye diseases such as glaucoma or retinopathy, which would make laser vision correction unsafe.
In such cases, the doctor explains the contraindications for vision correction surgery and guides the patient toward alternative options, such as prescription glasses, contact lenses, or certain tailored surgical procedures that are safer for their specific condition.
Irregular Corneal Topography
Corneal topography is one of the key tests used to determine whether you are a suitable candidate for laser vision correction.
When corneal topography shows irregular findings, this indicates an abnormality in the shape or thickness of the cornea, such as early keratoconus or localized thinning in specific areas.
In such cases, laser vision correction procedures like LASIK or Femto-LASIK are considered unsafe, as they may further weaken the cornea and increase the risk of serious complications such as post‑operative corneal ectasia.
For this reason, irregular corneal topography is regarded as one of the main contraindications to laser vision correction. In these situations, the ophthalmologist will often recommend alternative options, such as rigid gas-permeable contact lenses, intracorneal ring segment implantation, or phakic intraocular lens (IOL) implantation instead of removing corneal tissue.
This test plays a crucial role in protecting the patient from undergoing an inappropriate procedure and in ensuring that the safest possible method is chosen for vision correction.
Reduced Corneal Sensitivity or Nerve Damage Due to Previous Disease
Reduced corneal sensitivity or damage to corneal nerves as a result of prior conditions—such as recurrent keratitis, severe dry eye disease, or chemical injuries—is an important factor that may render a patient unsuitable for laser vision correction.
Laser procedures depend on the integrity of the corneal surface and the health of the corneal nerves that regulate tear production and ocular surface sensation, especially since LASIK and Femto-LASIK can temporarily worsen dryness in the early postoperative period.
If the cornea is already hypoesthetic or the nerves are compromised, the risk of severe dry eye, corneal epithelial defects, ulceration, and delayed wound healing after surgery increases significantly.
Therefore, reduced corneal sensitivity is considered a contraindication to refractive laser surgery in many cases. The patient typically requires thorough evaluation with specific tests for corneal sensitivity and for assessing the severity of dry eye.
In such situations, the ophthalmologist may recommend treating the dry eye first, avoiding corneal surface laser procedures, and looking into safer alternatives such as spectacles, therapeutic contact lenses, or certain types of intraocular lenses, depending on the individual case.
Endothelial Dysfunction / Low Endothelial Cell Count
The corneal endothelium (endothelial cells) is the innermost layer of the cornea, responsible for maintaining its transparency and fluid balance.
When there is endothelial dysfunction or a significant reduction in the endothelial cell count, laser vision correction becomes more hazardous, as any additional stress on the cornea may lead to persistent edema and loss of transparency.
Endothelial cell density is measured using a specialized test (specular microscopy). If the endothelial cell count is found to be below the normal range, this is considered a relative or even absolute contraindication to corneal laser procedures—particularly in patients with conditions such as Fuchs endothelial corneal dystrophy.
As part of the preoperative assessment for refractive surgery, the ophthalmologist carefully evaluates the endothelium to ensure that the cornea can tolerate surgical or laser intervention without compromising long‑term clarity.
If endothelial weakness is confirmed, the patient is usually advised to consider alternative methods for vision correction, such as glasses, contact lenses, or certain types of phakic intraocular lenses, along with regular follow‑up to monitor corneal health and preserve visual function.
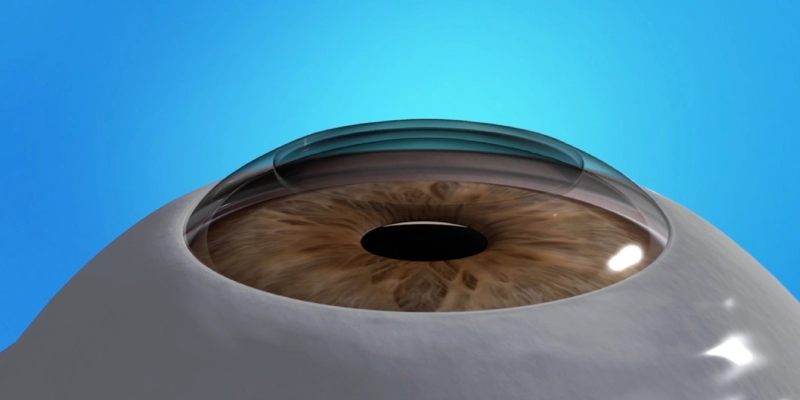
What alternatives are available for patients who are not suitable candidates for LASIK?
For patients who are not ideal candidates for LASIK vision correction—whether due to thin corneas, very high degrees of myopia or hyperopia, or chronic dry eye—there are several safe and effective alternatives. These include ReLEx SMILE (Small Incision Lenticule Extraction), phakic intraocular lens implantation (ICL), surface laser procedures such as PRK (Photorefractive Keratectomy), as well as advanced prescription contact lenses.
Phakic IOLs are particularly useful for patients with high levels of astigmatism or significant refractive errors that fall outside the safe range for LASIK. In this procedure, a specially designed lens is implanted inside the eye without removing the patient’s natural crystalline lens.
Surface laser treatment (PRK) is often recommended for patients with thin corneas who are not good candidates for creating a corneal flap, as is done in conventional LASIK. Although visual recovery with PRK may take longer, it offers stable and predictable long‑term visual outcomes.
In situations where any form of refractive surgery is not advisable, high‑precision prescription glasses, or daily and monthly disposable contact lenses, remain safe and effective options for vision correction and for improving visual quality.
Selecting the most appropriate alternative to LASIK requires a comprehensive assessment by an ophthalmologist, including corneal evaluation, measurement of the refractive error, and an overall review of ocular health, to ensure the best possible outcome with maximum safety.
Surface Laser (PRK)
Photorefractive keratectomy (PRK) is one of the most important alternatives for patients who are not suitable candidates for LASIK, particularly in cases of thin corneas or when corneal thickness issues make creating a corneal flap in conventional LASIK unsafe.
In PRK, a very thin superficial layer of the cornea is removed instead of creating a flap, then an excimer laser is used to reshape the corneal surface and correct refractive errors such as myopia, hyperopia, and astigmatism.
PRK reduces flap‑related complications such as flap displacement or inflammation, which makes it a suitable option among vision correction alternatives for patients who have contraindications to LASIK.
Recovery after PRK can be somewhat longer than after LASIK, with possible pain or burning sensation in the first few days, but the final outcomes are usually stable and excellent in terms of visual clarity and quality.
It is advisable to discuss with your ophthalmologist whether PRK is a safe and appropriate option for vision correction in the presence of LASIK contraindications or a history of corneal injury.
SMILE (Small Incision Lenticule Extraction) in Selected Cases
Small Incision Lenticule Extraction (SMILE) is a modern technique for vision correction and can be an appropriate alternative for some patients who are not good candidates for conventional LASIK, especially those with moderate to high myopia and adequate corneal thickness.
SMILE relies on a femtosecond laser to create a small lenticule inside the cornea, which is then removed through a very small incision, without the need to lift a large corneal flap as in LASIK, thereby better preserving corneal strength and biomechanical stability.
SMILE can be preferable for patients with dry eye or those concerned about flap‑related complications in LASIK, as this technique causes less disruption of the corneal surface nerves and may therefore reduce the severity of postoperative dry eye.
However, SMILE is subject to specific indications and is not suitable for all refractive errors or high degrees of astigmatism. Corneal thickness and the degree of refractive error must be carefully evaluated before choosing it as a LASIK alternative.
Including SMILE among vision correction options helps patients with LASIK contraindications find a safe and effective solution that improves vision and reduces dependence on glasses and contact lenses.
Implantable Collamer Lens (ICL) as a Safe Alternative
Implantable Collamer Lenses (ICL) are among the safest alternatives for patients who are not candidates for LASIK or for any corneal laser procedures, such as those with very thin corneas or extremely high refractive errors.
In this technique, a thin, transparent lens is implanted inside the eye between the iris and the natural crystalline lens without removing any part of the cornea, thus preserving corneal structure and reducing the risk of biomechanical weakening or later development of keratoconus.
ICL lenses are used to correct high myopia and, in some models, hyperopia and astigmatism. They provide high‑quality vision and can be removed or replaced in the future if necessary, making them a flexible option for patients with LASIK contraindications.
These lenses are an ideal choice for younger patients who do not wish to undergo clear lens extraction, and for individuals who are not suitable for corneal laser correction due to corneal thickness or shape.
Choosing ICL implantation as a refractive option should only be made after thorough examinations of ocular measurements, intraocular pressure, and anterior chamber depth to ensure safety and achieve the best possible visual outcome.
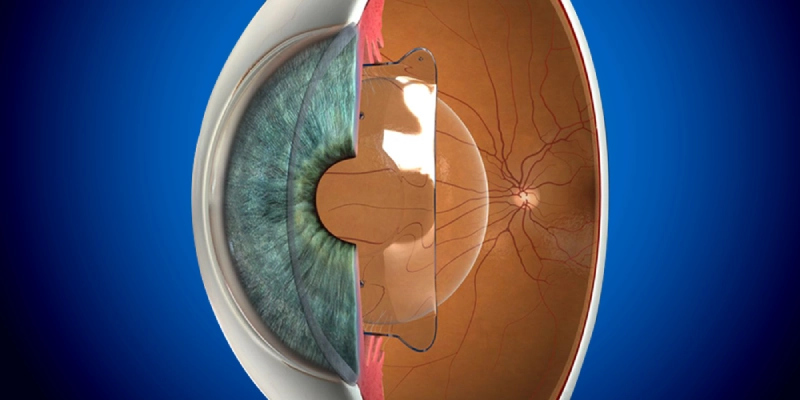
Corneal Cross-Linking (CXL) for Keratoconus
Corneal collagen cross-linking with ultraviolet light and riboflavin (CXL) is not a direct vision correction procedure, but it is a crucial step for patients who are not suitable for LASIK because of keratoconus or weakened corneal structure.
CXL strengthens the corneal collagen fibers by soaking the cornea with riboflavin (vitamin B2) and then exposing it to ultraviolet light, which increases cross-links between collagen fibers and thereby enhances corneal rigidity and stability.
This procedure helps halt or slow the progression of keratoconus, protecting patients from continued visual deterioration and potentially allowing the later use of specialty contact lenses or additional procedures to improve visual acuity.
In the context of contraindications to laser vision correction, detecting keratoconus or early signs of it is one of the main reasons to refuse LASIK, and this is where CXL emerges as a fundamental preventive treatment to preserve the cornea.
CXL can sometimes be combined with other procedures, such as intracorneal ring segment implantation or the use of specialty lenses, with the aim of maximizing visual improvement while ensuring long‑term corneal stability.
How can you be sure you’re not a candidate for vision correction surgery?
The only reliable way to know you’re not suitable for laser vision correction is through a comprehensive evaluation by an ophthalmologist who specializes in refractive surgery. This assessment typically includes measuring corneal thickness, checking the stability of your prescription, and examining the health of the cornea, retina, and any underlying chronic eye conditions.
You are often considered unsuitable for LASIK, femto-LASIK, or surface ablation procedures (such as PRK) if you have a thin or keratoconic cornea, severe dry eye that does not respond to treatment, active autoimmune or inflammatory diseases, are pregnant or breastfeeding, or if your prescription has continued to change over the past 12 months.
Your surgeon may also advise against laser vision correction if you are taking medications that interfere with corneal healing, or if you have a history of significant eye infections or complex ocular surgeries.
Real certainty does not come from symptoms alone or from online information. It requires specialized tests such as corneal topography, corneal pachymetry (thickness measurement), and a detailed fundus examination. Based on these findings, your ophthalmologist can safely determine whether you have any contraindications to refractive surgery and, if so, recommend safer alternatives such as glasses, contact lenses, or other surgical options when appropriate.
Book Now at Batal Specialized Center to Check Your Eligibility for Vision Correction Surgery
If you’re considering laser vision correction, the first and most important step is to schedule a specialized consultation to assess your eyes and determine whether you’re a suitable candidate for the procedure.
At Batal Specialized Center, our team of ophthalmology consultants provides a comprehensive evaluation that includes:
- Visual acuity testing
- Corneal thickness measurement (pachymetry)
- Retinal examination
- Screening for medical contraindications such as keratoconus, severe dry eye disease, or autoimmune disorders that may affect corneal healing
This thorough assessment helps identify the safest and most effective vision correction options for your specific condition, while minimizing the risk of potential complications. You’ll also receive clear, detailed answers to all your questions regarding the safety of the procedure and the expected outcomes.
Book your appointment now at Batal Specialized Center to ensure your eyes are healthy and confirm your eligibility for vision correction surgery before making your final decision.

Frequently Asked Questions About LASIK Contraindications
1. Who is not a candidate for LASIK or laser vision correction?
You may not be a good candidate for LASIK if you have keratoconus or other corneal ectatic disorders, very thin corneas, advanced retinal disease, uncontrolled glaucoma, severe dry eye, or active autoimmune or inflammatory conditions. In these cases, laser vision correction may be unsafe or may not provide meaningful visual improvement.
2. Does keratoconus permanently rule out laser vision correction?
Yes. Keratoconus and other corneal ectasias are generally considered permanent contraindications to LASIK and similar procedures. Laser treatment on a structurally weak cornea can accelerate ectasia, worsen irregularity, and significantly reduce visual quality.
3. Can I have LASIK if I have thin corneas?
If your cornea is below the safe thickness threshold, LASIK is usually not recommended because removing tissue with the laser can compromise corneal stability and increase the risk of post-LASIK ectasia. In such cases, your surgeon may suggest alternatives like PRK, SMILE in selected cases, or phakic intraocular lenses (ICL).
4. Are autoimmune diseases a contraindication to LASIK?
Poorly controlled autoimmune diseases such as lupus, rheumatoid arthritis, or severe psoriasis can interfere with corneal healing and increase the risk of infection, inflammation, and visual complications after surgery. Many surgeons therefore avoid LASIK in these patients or postpone it until the disease is well controlled in coordination with the treating specialist.
5. Is LASIK safe for patients with diabetes?
Diabetes that is well controlled and without significant diabetic retinopathy may be compatible with refractive surgery in some cases. However, poorly controlled diabetes or advanced diabetic retinopathy can cause unstable prescriptions and delayed corneal healing, making laser vision correction unsafe or inappropriate until the condition is stabilized.
6. Why are pregnancy and breastfeeding temporary contraindications to laser vision correction?
During pregnancy and breastfeeding, hormonal changes can affect corneal thickness, curvature, and tear film stability, causing temporary shifts in refraction. Performing LASIK during this period can lead to inaccurate results and the need for enhancement later, so surgery is usually postponed until several months after breastfeeding has ended.
7. What tests are used to determine whether I am a suitable candidate for LASIK?
A comprehensive preoperative evaluation typically includes visual acuity testing, refraction, corneal topography and tomography, corneal thickness measurement (pachymetry), intraocular pressure measurement, and a dilated fundus examination. These tests help identify issues such as thin or irregular corneas, keratoconus, glaucoma, or retinal disease that may contraindicate surgery.





