Keratoconus surgery
Keratoconus surgery
Keratoconus is one of the eye diseases that cannot be corrected by LASIK (which is suitable for treating many eye problems). It is a disease that affects the normal shape of the cornea of the eye so that the cornea becomes conical and protrudes significantly outward, causing poor vision as well as affecting the aesthetic appearance of the eye.
Signs and symptoms of keratoconus
When infected with keratoconus, the transparent lens surrounding the eye gradually thins and thus leads to the appearance of a cone-shaped bulge and ultimately leads to impairment of the eye’s ability to focus properly, causing weak and blurry vision, severe sensitivity to light, double vision, weakness or no night vision, and rapid decline in The strength of vision is such that you need to change the size of the glasses frequently in a short period of time.
Causes of keratoconus
The exact cause is unknown. It affects the 18 to 22 age group and causes changes in the shape of the cornea of the eye every year until the 30s and 40s, and the eyes protrude at a faster rate in younger patients. Keratoconus rarely affects children or the elderly and may appear in one or both eyes.
There is no specific and clear cause of keratoconus, but some studies say that excessive rubbing of the eyes, the wrong use of contact lenses, chronic eye irritation, and exposure to UV rays may be among the factors that contribute to the appearance of keratoconus.
The effect of keratoconus
Often, visual acuity is not affected in the early stages of keratoconus, and as the condition develops, the external eye shape is affected more and the thinning state increases, which impairs the eye’s ability to focus, increases sensitivity to light and decreases visual acuity significantly. So what are the options for treating keratoconus?
Keratoconus treatment
Keratoconus does not need urgent surgery because the changes it causes to the cornea of the eye usually take months and years before the condition worsens, and that is why we recommend regular follow-up (every 6 to 12 months) and re-tests of vision and refraction (ophthalmometry) and corneal examinations for up to five years since The start of case detection.
Keratoconus is known to cause fluctuations in vision and these fluctuations do not usually indicate a change in the condition. We recommend consulting a doctor if there is a deterioration in vision, but fluctuation does not mean that there has been a change in the degree of convexity. And each degree is treated as follows.
Soft Lenses
Usually, vision can be corrected even in the later stages of the injury. The treatment at Batal Eye Specialist Complex varies according to the stage. In the first stage, the doctor can prescribe glasses and soft contact lenses to correct vision in mild to moderate cases.
Hard Lenses
As the condition progresses and the degree of corneal thinning and steepening increases, the trend is towards rigid gas permeable lenses to correct vision. Rigid lenses are one of the most effective treatments for keratoconus because they gently reshape the cornea of the eye into its proper circular shape, thus improving vision.
Attaching contact lenses to keratoconus is not an easy and time-consuming process, and you may need to visit your doctor more than once so that he can adjust it to the correct size.
Corneal fixation
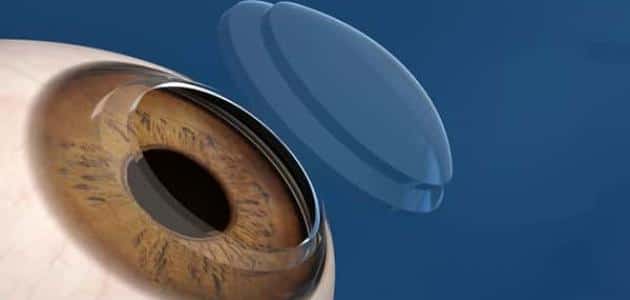
Keratoplasty is an appropriate treatment for keratoconus if the lenses do not help correct vision, because this operation changes the shape of the eye’s cornea to a natural circular shape that allows normal vision to return. This operation does not cure the effects of keratoconus that have already occurred, but it stops the deterioration of the condition and prevents access to the conical shape of the eye. The patient may need to wear contact lenses or glasses even after corneal fixation surgery.
Protecting the cornea with collagen
Corneal cross-linking surgery can effectively stop the progression of keratoconus and it involves a combination of collagen and riboflavin (vitamin B2), which are activated by ultraviolet light to significantly strengthen the corneal stiffness.
First, the top layer of the cornea (the epithelium) is gently removed, then the cornea is saturated with collagen and riboflavin, and a UV light is applied to activate the solution. Sometimes stopping the progression of keratoconus.
The procedure takes about one hour and is performed on an outpatient basis. Patients usually experience some mild discomfort in the immediate postoperative period. After treatment, the patient is fitted with a contact lens that remains in place for up to three days. Antibiotic drops are placed on the treated eye until the surface heals. This is followed by steroid drops for about 5 to 6 weeks.
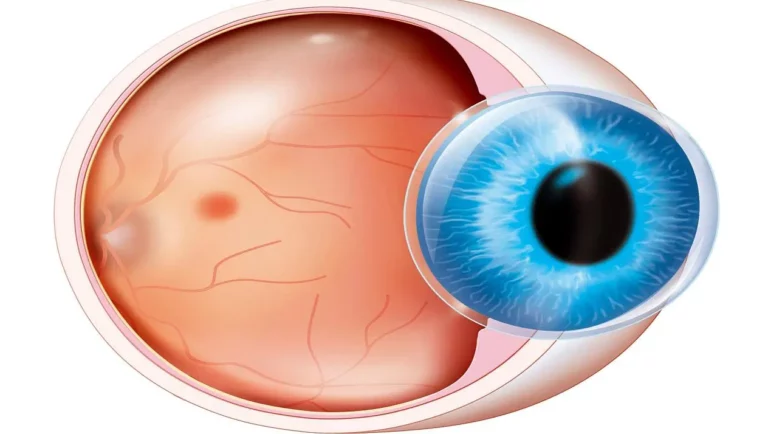
Corneal transplant (keratoplasty)
This will only be suggested if all other treatment options have been exhausted — about 10-20% of patients eventually require a corneal transplant. There are two types of corneal transplants: partial thickness and full thickness (or penetrating) and the latter is usually the one recommended for patients with keratoconus.
Corneal transplant is a complex procedure and requires admission to a day surgery and is generally performed under local anesthesia, with the option of sedation. During the procedure, the surgeon will cut out the abnormal part of the cornea and replace it with a donor cornea, which will be stitched in place. Later on, the stitches will be removed and it will grow back. Your corneal cells gradually grow and fuse into the donor tissue and full recovery from this type of keratoconus surgery may take up to a year. in this.
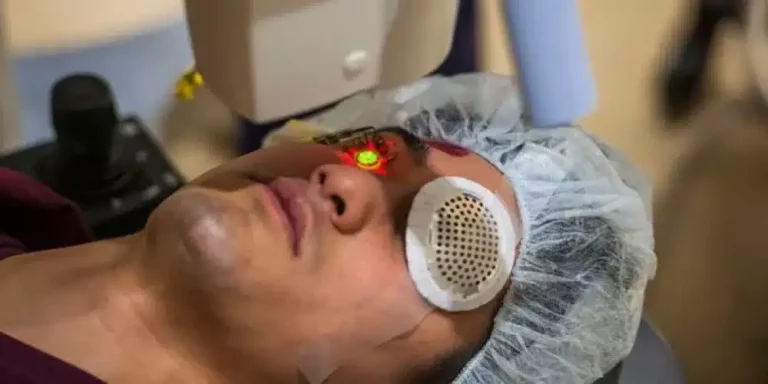
What does keratoconus surgery involve?
The patient returns home on the same day of the surgery, which is conducted as follows:
- The doctor begins numbing the eye with anesthetic drops, and the patient does not feel any pain.
- The doctor removes the thin, outer layer of the cornea to allow the drug to reach deep into the cornea.
- The doctor applies a special type of eye drop to straighten the cornea for 30 minutes.
- The doctor uses a special device to shine a focused beam of ultraviolet rays on the cornea for 30 minutes.
- The doctor places a contact lens pad over the eyes to aid healing and leaves it for about a week.
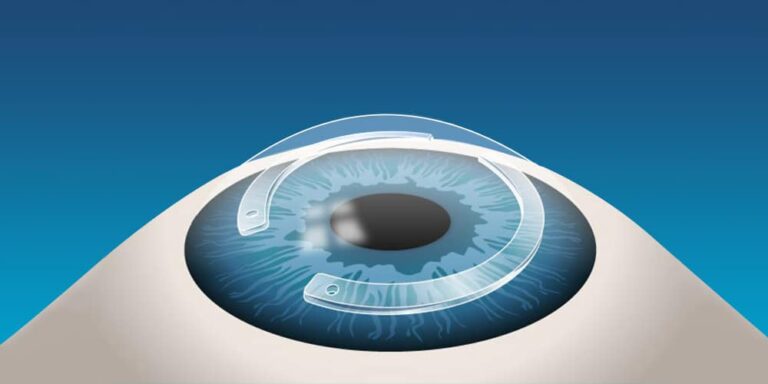
INTACS braces in the cornea of the eye
The ophthalmologist, through a surgical operation, places small arches inside the cornea that flatten and reshapes it, and vision improves as long as these brackets are in place, but vision will return to what it was before if these brackets moved or were removed. The use of a combination treatment of corneal fixation and bracket implants has shown good results in treating keratoconus.

Corneal transplant
Corneal transplantation is a rarely performed option and the doctor uses it in late cases and when the lenses do not give an adequate result due to cracks, severe thinning, or intolerance to contact lenses. The affected eye’s cornea is removed and replaced with a healthy one. This replacement may include a complete corneal replacement or only anterior or only posterior corneal tissue. It may take more than a year for vision to stabilize after a corneal transplant, and some people need special contact lenses after corneal transplantation to get the best vision.
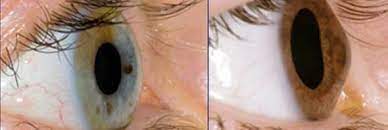
Diagnosis of Keratoconus at Batal Specialist Center
The ultimate goal of Batal Eye Specialist Complex doctors is to give our clients the best possible vision, whether keratoconus is in its early or late stages. Keratoconus can be difficult to diagnose in the early stages, and all symptoms indicating infection are similar to other eye diseases.
We have the latest diagnostic equipment, such as keratometry and topography, that monitor the initial signs of infection, follow the progression of the condition with great accuracy, and distinguish keratoconus from other diseases. Our physicians will discuss the treatment options available for each case.

Senior Consultant, Pediatric Surgery and Eye Surgery Fellow of the British Royal Surgical College Fellow of the American Academy of Ophthalmology
Specialization: Strabismus and pediatric eye surgery
Degree: Member of the British Royal College of Surgeons and Member of the American Academy of Ophthalmology
Batal Eye Center
Call us 8001111897
Contact us via Email: info@bataleyecenter.com
Address: 8125 Prince Sultan road, Murjana tower Jeddah, Saudi Arabia




