Electromyography of the retina and optic nerve
Electromyography of the retina and optic nerve
Retinal electromyography is one of the accurate eye examinations, and it is one of the most important methods of diagnosing serious eye diseases such as: night blindness, retinal detachment, optic neuritis, and other eye diseases that may lead to blindness and require urgent medical intervention.
At Batal Specialist Center, we focus on examining the electrocardiogram of the retina and the optic nerve in order to diagnose any sudden abnormality in the retina. This test translates electrical signals from the retina and optic nerve into data for the doctor to see, to determine the extent of the retina damage and to monitor any changes in the function of the retina or the optic nerve.
Does night blindness cause blindness?
Malfunction of the optic nerve or retina leads to serious complications, including blindness. These complications need to be quickly diagnosed and treated by our specialist team to stand the best possible chance of your sight being saved.
Night blindness
- Night blindness occurs as a result of a defect in the functions of the retina with which a person cannot see at night or in low light during the day as well, and among its symptoms is the difficulty of adapting the eyes when moving from a bright place to a dark place. It is common among those who suffer from short-sightedness. And we can detect this type of disease using the electrophoresis technique.
Diagnosis of night blindness
Prevention of night blindness
Night blindness treatment
The treatment for night blindness depends mainly on the cause of the night blindness, as it may be due to myopia. Here, the treatment is as simple as obtaining new glasses (a new size), and it may require surgical intervention if it is caused by another disease such as a cataract.
The treatment depends on the diagnosis of the disease that caused the appearance of night blindness if there was an injury to the retina that led to the emergence of the symptoms of night blindness, in this case, the person needs an additional examination by a retina specialist before determining the treatment.
The ophthalmologist at Batal will perform a comprehensive eye examination and request specialized x-rays and examinations before resorting to refractive surgeries such as LASIK and PRK that help change the shape of the cornea and thus improve vision.
And because night blindness is, in fact, a symptom of a number of other eye diseases, which often affect the retina (such as cataracts, myopia, vitamin A deficiency, or retinitis pigmentosa) and not a disease in itself, its treatment depends on determining the cause that may be one Of the following:
- Glaucoma disease or glaucoma medications: Glaucoma disease itself may be the cause of night blindness. In this case, treating the disease itself through eye drops, laser therapy, or surgery will improve vision, but the basic idea here is that the glaucoma drugs themselves may cause poor vision at night or in low light, so the treatment must be changed.
- Myopia: The degrees of myopia vary with time, and this can be observed when feeling blurred vision at night or in low-light rooms, which makes a person think that he has night blindness, but it is in fact not the case, and the treatment here is to change the size of the glasses or contact lenses to suit the degree of shortness Looking new.
- Cataracts: The lens of the eye is weakened and night vision is blurred due to aging. The treatment we recommend here is cataract surgery or cataract surgery and replacing the eye’s natural cloudy lens with a new one, so your vision will improve both during the day and at night as well.
- Refractive eye surgery: If you get night blindness after LASIK surgery or PRK surgery, you should consult your ophthalmologist about adding an anti-reflective coating to your lenses to reduce glare and improve vision.
- Diabetes: The doctor will determine here whether Diabetic Retinopathy is the cause of the night blindness, and accordingly, the treatment will be determined by either medication, surgery, or laser.
- Vitamin A deficiency: The cause of night blindness may not be as dangerous as in the previous cases and be due to a deficiency of vitamin A that affects vision, all that is needed is to eat foods that contain vitamin A and nutritional supplements prescribed by the doctor.
- Genetic factors: If night blindness is caused by genetic factors or from retinitis pigmentosa that scientists have not yet discovered a cure for, you can talk to one of our doctors about how to cope with night blindness and reduce the risk of accidents.
Retinal detachment
Retinal detachment occurs when the retina separates from its basic structure (the back of the eye) due to fluid accumulation behind the retina. Retinal detachment is often painless. There are many causes of retinal detachment, but the most common are aging and eye injuries. An eye injury may result from a serious injury or after an eye surgery such as cataract surgery. The risk of retinal detachment also increases in myopic people between the ages of 25 and 50.
And because retinal detachment is a dangerous condition that may lead to temporary or permanent blindness, we recommend that at Batal Eye Specialist Center, consult an ophthalmologist immediately after exposure to an eye injury or feeling any of the symptoms of retinal detachment, because early treatment helps prevent vision loss. We also recommend regular comprehensive eye exams, especially for those who suffer from severe nearsightedness. At Batal Medical Center, we offer the electromyography technique of the retina and the optic nerve, and this technique is important in diagnosing this disease.
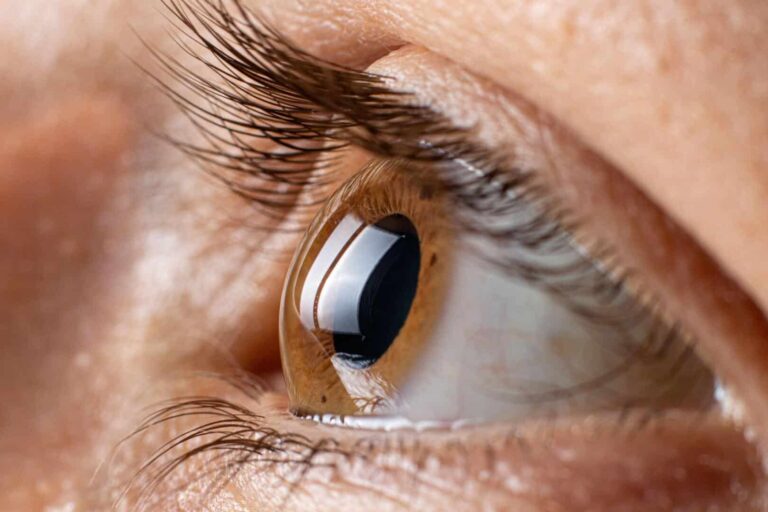
Understanding retinal detachment
Seeing a few small dark spots or zigzag lines is normal and not alarming, but the main complaint of patients diagnosed with a detachment of the retina is seeing these spots and lines frequently and suddenly, in addition to feeling as if there is a cloud over the eye obscuring the vision. If this happens suddenly and more than usual and the eyes continue to blink or blurry vision, you should consult your doctor immediately, as this may be an early warning of retinal detachment.

Laser treatment of retinal detachment
After performing the necessary tests and determining the degree of retinal detachment, the doctor decides whether cryotherapy or laser treatment of retinal detachment is appropriate for the case. Our message that we want to send here is to reassure our patients, as treatment for retinal detachment works for 9 out of 10 people.

Optic neuritis
Optic neuritis causes sudden blindness that may be complete or partial, and it also causes pain in the eyeball that often occurs with eye movement, and leads to a defect in color vision, and the condition affects young people in middle age and women more than men.
Damage to the optic nerve may result from glaucoma or any serious disease of the retina. Certain chemicals, medications, or nutritional deficiencies can cause inflammation or damage to the optic nerve. Improvement occurs if we treat the underlying cause in a timely manner with appropriate treatment.
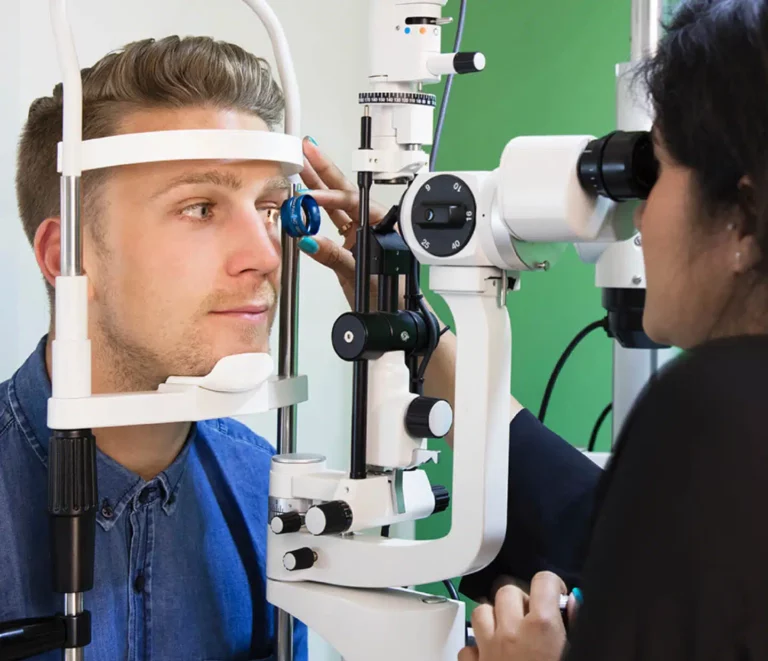
Optic nerve examination
Optic neuritis affects vision and it may turn from just inflammation to atrophy and damage to visual tissues when treatment is neglected and thus vision is lost within days, and optic neuritis may not lead to vision problems in its early stages, and the symptoms are similar to other diseases that may affect the eye. Accordingly, the doctor will order accurate tests and examinations.
Diagnosis of optic neuritis at Batal Eye Specialist Center is done through a comprehensive medical examination, examination of the fundus, and evaluation of the eye’s response to light. The ophthalmologist may need an MRI scan of the brain in some cases to make sure of its diagnosis, knowledge of the treatment plan, and whether the condition really requires treatment with an anti-inflammatory or if the inflammation will disappear on its own.
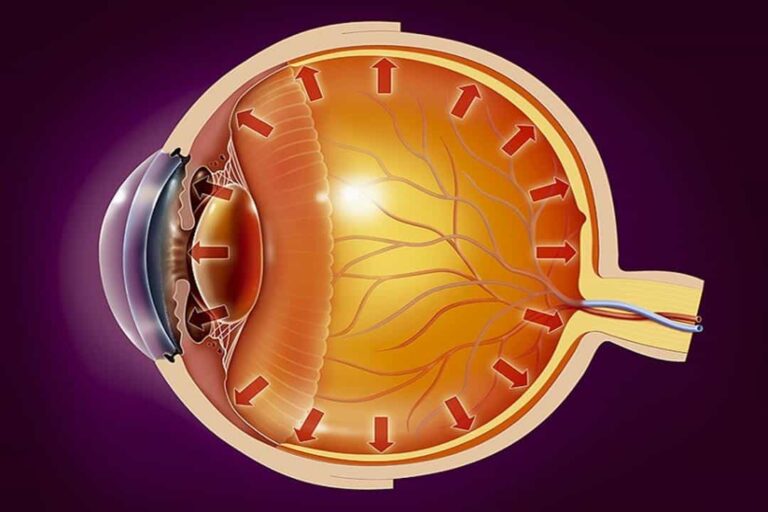
Optic nerve and eye pressure
Blockage of the tear ducts causes eye pressure to rise to high levels, and if eye pressure remains high for a long time, this will lead to atrophy of some of the retinal nerve fibers and may end in blindness. Here, we find that the diagnosis of glaucoma depends largely on measuring intraocular pressure, in which case the first line of tracking treatment for optic neuritis is the treatment of glaucoma mainly.
Vision loss occurs in the late stages of glaucoma, but successful treatment prevents vision deterioration. Therefore, we strongly advise at Batal Specialist Center to diagnose the disease in its early stages as much as possible and to conduct glaucoma diagnostic tests that rely heavily on measuring intraocular pressure.
The medical treatment for glaucoma currently consists of using eye pressure drops. If the intraocular pressure remains high after drug treatment, surgical intervention or laser operations are preferred.

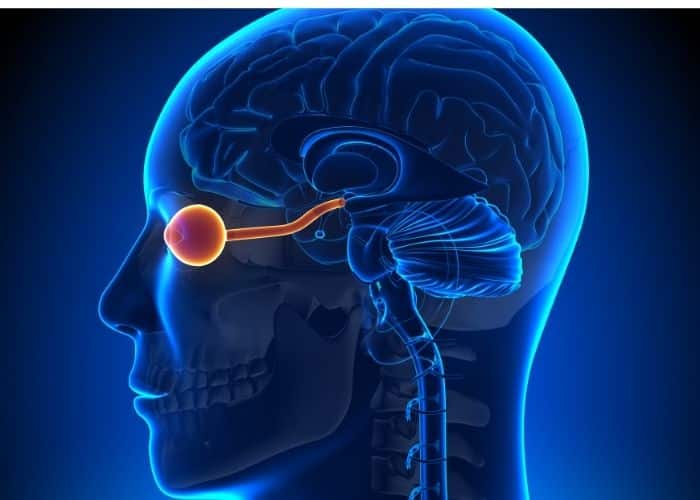
The relationship between the optic nerve and the retina
The optic nerve is located in the center of the retina and the optic nerve carries the impulses made by the retina to the brain. Damage to the optic nerve can cause a number of diseases of the retina. The danger of optic neuritis is that its symptoms appear suddenly and the condition deteriorates within a few days after the onset of symptoms, but the good news is that the correct treatment gives effective results within 4 to 6 weeks in most cases.
Patients tell us that our attention to detail, advice and guidance makes them satisfied with the medical service they have received. You can get our services by booking an appointment by contacting us on our visible numbers or through our pages on social media, or by subscribing to the patient service on WhatsApp.
Overview of electrophysiological tests of the eyes
Vision is the result of electrical signals that travel between the retina and the part of the brain associated with vision. Electrophysiology tests check to see how well the optic nerve pathway sends these electrical signals necessary for vision. These tests measure the electrical activity that occurs in the eye when looking at something.
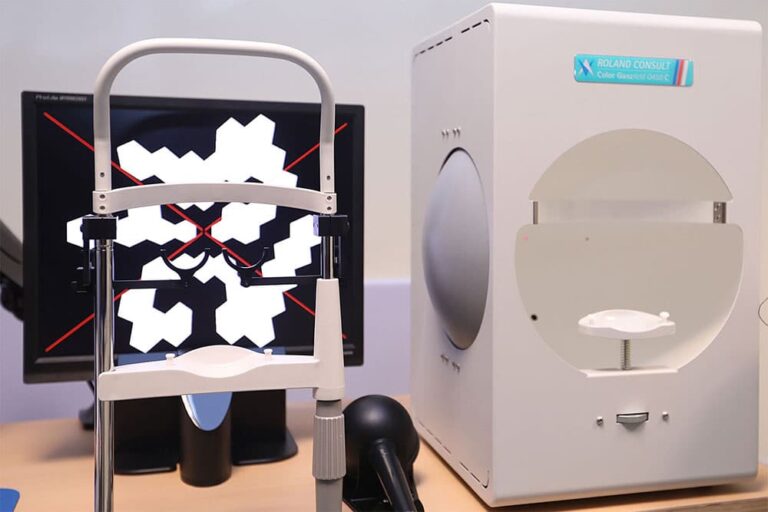
Electroretinography (ERG)
Full-field ERG measures the electrical response of the retina while looking at different patterns or flashes of light and measures how well the cone cells are functioning and helps these cells detect light and color and also checks for other cells in the retina and can be used to check for problems such as:
- CoDamage to the retina from medications or other substances.
- Night blindness (difficulty seeing in low light).
- Eye problems due to vascular disease.
The multifocal ERG tests the electrical response in the central part of the retina and may be used to help check the following:
- Macular diseases that are not found by full-field ERG
- Unexplained central vision loss not found by whole field ERG.
- Some types of retinitis pigmentosa.
How is it done:
- Sit or lie down during the test.
- Use eye drops to numb the eye
- A small electrode is placed in front of the eye and on the face
- Looking at a screen that displays flashes of light, the test records the electrical response and shows the electrical activity of the eye on a machine called an oscilloscope
- The test is done in light and dark.
- The total scan takes about an hour.

Electrooculogram (EOG)
An EEG tests how well electrical currents are working in the entire eye and is done to check for certain eye and retinal problems and can be used to help check for problems such as retinal diseases such as congenital macular degeneration and retinitis pigmentosa.
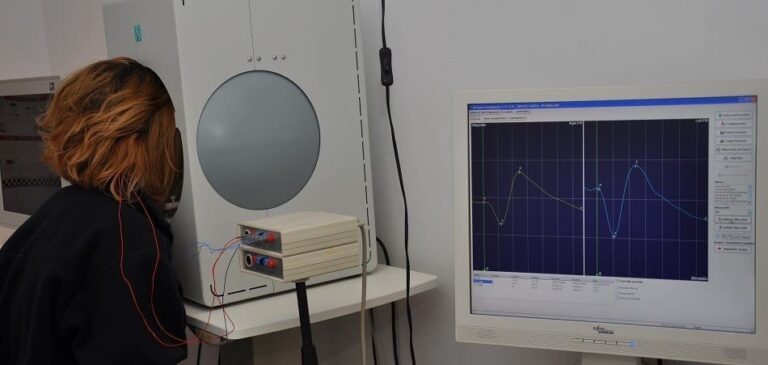
Visual Evoked Response (VER or VEP)
The visual evoked response tests the electrical activity in the entire visual pathway from the eyes to the parts of the brain associated with vision. This test measures electrical activity when the eye responds to looking at an object. Testing can detect problems by showing how your brain waves respond to certain objects you look at during the test.
How to prepare
There is no need to do anything special to prepare for the test as you should just follow the instructions of the Champion Specialist Center on what to do before the test:
- Follow your doctor’s eating instructions to avoid low blood sugar.
- Avoid caffeine within 12 hours of the test.
- Wash hair well before testing.
- Do not wear any jewelry near the head.


These tests usually cause little or no discomfort.
A person may not be able to perform the tests or the results may not be useful when instructions cannot be understood or followed. For example, some vision tests cannot be performed on infants, young children, or people who cannot understand or follow instructions. Taking the test or it may change the results of the test. Therefore, you must visit the Eye Center in Al-Batal Specialized Complex in Jeddah about the reasons for conducting this test and what the results mean.

Senior Consultant, Pediatric Surgery and Eye Surgery Fellow of the British Royal Surgical College Fellow of the American Academy of Ophthalmology
Specialization: Strabismus and pediatric eye surgery
Degree: Member of the British Royal College of Surgeons and Member of the American Academy of Ophthalmology
Batal Eye Center
Call us 8001111897
Contact us via Email: in**@************er.com
Address: 8125 Prince Sultan road, Murjana tower Jeddah, Saudi Arabia



