Med info
Vision Correction: A Complete Guide to Requirements, Procedures, Technologies, and Safety in 2026

What Is Vision Correction and How Does It Work?
Vision correction refers to a range of medical procedures and optical techniques designed to improve visual acuity and treat refractive errors such as myopia (short-sightedness), hyperopia (long-sightedness), astigmatism, and presbyopia (age‑related difficulty focusing on near objects).
These methods work by properly focusing light rays onto the retina instead of allowing them to fall in front of it or behind it, which results in clearer, sharper vision.
This can be achieved in several ways, including prescription eyeglasses, contact lenses, or laser eye surgeries such as LASIK, Femto-LASIK, and surface ablation procedures (like PRK and similar techniques).
Such interventions either reshape the curvature of the cornea or compensate for the refractive error using tailored lenses, which can reduce or sometimes eliminate the need for glasses and improve the patient’s overall quality of life.
When appropriately indicated, vision correction surgeries are among the most common and effective solutions for treating widespread vision problems, provided that the case is thoroughly evaluated by a qualified ophthalmologist before choosing the most suitable option.

What conditions require vision correction?
Vision correction becomes necessary when certain visual problems appear, such as:
- Myopia (short-sightedness), which makes it difficult to see distant objects clearly.
- Hyperopia (long-sightedness), which affects the clarity of near vision.
- Astigmatism, which causes blurred or distorted vision at all distances due to an irregular curvature of the cornea or lens.
Many people also start needing vision correction after the age of forty because of presbyopia (age‑related difficulty with near vision), which makes tasks like reading or using a smartphone up close more challenging.
Procedures and tools such as laser vision correction (e.g., LASIK, PRK), contact lenses, or prescription glasses are often recommended when there is:
- Recurrent headache related to eye strain
- Difficulty driving at night
- Reduced visual concentration during studying or work
In specific situations—such as a significant difference in refractive power between the two eyes (anisometropia) or the presence of misalignment in the visual axis (strabismus or certain axis deviations in astigmatism)—vision correction becomes essential to maintain binocular balance, prevent deterioration, and improve overall quality of daily life.

Who is the best candidate for vision correction surgery? (Key eligibility criteria)
The ideal candidate for vision correction surgery is an adult with nearsightedness (myopia), farsightedness (hyperopia), or astigmatism, whose prescription has been stable for at least one to two years without significant change in their eyeglasses or contact lenses.
In most cases, the patient should be over 18 years of age, in generally good health, and free of poorly controlled chronic conditions such as uncontrolled diabetes or autoimmune diseases.
The cornea must be structurally healthy, with adequate thickness and a normal shape, and free of keratoconus or significant thinning. This is confirmed through advanced preoperative tests before laser vision correction procedures such as LASIK or PRK.
It is also preferable that the patient does not suffer from severe dry eye or recurrent eye infections, and that there are no underlying retinal diseases or optic nerve problems that could compromise visual quality after surgery.
Most importantly, the candidate should have realistic expectations regarding the outcome of vision correction surgery and be willing to follow all pre- and postoperative instructions carefully, in order to achieve the best possible and most stable long-term visual results.
Appropriate Age for Laser Vision Correction
Age is one of the key factors in determining who is a good candidate for laser vision correction.
Surgery is generally recommended after the age of 18–21, when the refractive error (myopia, hyperopia, or astigmatism) has usually stabilized.
Most ophthalmologists require the prescription to be stable for at least one to two years before considering any refractive procedure. If the prescription continues to change after surgery, the visual outcome may be less stable and the patient may need glasses again or a secondary enhancement procedure.
In older adults, each case is assessed individually, taking into account additional issues such as early cataract formation, dry eye disease, or corneal pathology.
Therefore, there is no single “ideal age” for laser vision correction; the timing depends on refractive stability and overall ocular health, best determined through a thorough examination by a refractive eye surgeon.
Required Corneal Thickness
Corneal thickness is a critical parameter in selecting suitable candidates for refractive surgery, especially LASIK and surface ablation procedures such as PRK.
The surgeon needs an adequately thick cornea (on average around 500–550 microns) to safely remove a calculated amount of corneal tissue while preserving a sufficient residual stromal bed after surgery.
If the cornea is thin or below the surgeon’s safety threshold, conventional LASIK may not be advisable. In such cases, alternatives like surface ablation (PRK) or implantable collamer lenses (ICL) and other intraocular lens-based procedures may be considered.
Corneal pachymetry and tomography (e.g., Pentacam and similar devices) are essential steps in evaluating eligibility for laser vision correction, as they help minimize risks such as postoperative corneal weakening or iatrogenic keratoconus (ectasia).
Thus, candidacy is not based solely on the glasses prescription; precise corneal measurements are needed to ensure that refractive surgery outcomes are safe and stable in the long term.
Refractive Error Range Suitable for Surgery
The degree of myopia, hyperopia, and astigmatism plays a major role in determining who is an appropriate candidate for laser vision correction.
LASIK and surface ablation techniques are typically suitable for mild to moderate myopia and in some cases higher myopia, often up to approximately −1.00 to −8.00 or −10.00 diopters, depending on the surgeon’s assessment and corneal thickness.
Hyperopia usually has a narrower effective treatment range with laser procedures, commonly up to about +4.00 or +5.00 diopters, provided the prescription is stable and there are no corneal abnormalities.
Various degrees of astigmatism can also be corrected within defined limits, but confirming a regular corneal surface with detailed corneal topography is essential before proceeding.
All these numbers are approximate and may vary between centers and individual patients. A comprehensive eye examination is therefore indispensable, because the “ideal prescription for surgery” depends not only on the diopters, but also on corneal integrity, pupil size, and the health of the retina and optic nerve, to ensure safe and effective freedom from glasses and contact lenses.

Cases in Which Surgery Is Not Recommended
Although refractive surgery is an effective solution for reducing or eliminating dependence on glasses and contact lenses, it is not suitable for everyone. In some situations, it is not recommended in order to protect the health of the eye.
Key contraindications include frank keratoconus or suspected forme fruste keratoconus, and markedly thin corneas that cannot safely tolerate adequate tissue removal.
Surgery is also discouraged when the refractive error is unstable, in cases of rapidly progressing myopia, or in the presence of certain retinal or optic nerve diseases that may limit visual potential even after optical correction.
In addition, refractive surgery is generally not advised in patients with active autoimmune disease, severe or uncontrolled dry eye, recurrent ocular infections, or during pregnancy and breastfeeding in many cases, due to hormonal changes that can affect the cornea and refractive status.
Accurate identification of these situations helps ensure that only appropriate candidates undergo refractive surgery, avoiding unnecessary risk and unstable outcomes, and underscores the importance of a thorough, individualized medical evaluation before deciding on surgery.
Preoperative Tests Before Laser Vision Correction
Before undergoing laser vision correction, ophthalmologists request a series of detailed tests to ensure the eyes are healthy and that the patient is a suitable candidate for surgery.
These assessments typically include measuring visual acuity using standard eye charts, as well as determining corneal thickness (pachymetry) to confirm that the cornea can safely tolerate the removal of microscopic layers during LASIK or Femto-LASIK procedures.
Corneal topography is also performed to create a detailed map of the corneal surface and to detect any irregularities or signs of keratoconus, which could make laser vision correction unsafe.
In addition, intraocular pressure is measured (tonometry) to rule out elevated eye pressure or early glaucoma, and a thorough fundus and retinal examination is carried out to ensure there are no underlying retinal or optic nerve conditions that might affect the surgical outcome.
Together, these comprehensive tests help determine the most appropriate type of vision correction procedure, minimize the risk of complications, and support long-term stability of visual results.
Corneal Thickness Measurement (Pachymetry)
Corneal pachymetry is one of the most important preoperative assessments before vision correction procedures, to ensure both the safety and effectiveness of surgery.
This test accurately measures corneal thickness in microns, which is a key factor in determining the most suitable refractive technique, such as LASIK, Femto-LASIK, or PRK.
If the cornea is thinner than normal, the risk of complications such as postoperative corneal instability (ectasia) increases. Measuring corneal thickness helps avoid these risks and assists in choosing the safest and most appropriate treatment plan.
Pachymetry also helps precisely calculate how much corneal tissue will be ablated by the laser, leading to more accurate correction of myopia, hyperopia, and astigmatism.
This quick, painless test is an essential step for anyone considering laser vision correction, and it provides the ophthalmologist with critical information to make a safe, individualized decision for each patient.
Corneal Topography
Corneal topography is a three-dimensional mapping of the shape and curvature of the corneal surface, and is a cornerstone test before any form of laser vision correction.
It allows the detection of any irregularities on the corneal surface, such as early keratoconus or subtle abnormalities that may not be visible on routine examination, and that could make the patient unsuitable for certain types of LASIK procedures.
By using corneal topography, the ophthalmologist can tailor a customized vision correction plan for each eye and choose the optimal technique to achieve the best possible visual acuity while minimizing postoperative glare and halos, especially at night.
This test is also used to monitor corneal stability over the long term after refractive surgery, making it a fundamental part of assessing the safety and long-term success of the procedure.
If you are considering laser vision correction, corneal topography helps ensure that your corneal surface is suitable for surgery and that your visual outcome is likely to be stable and precise.
Dry Eye Evaluation
Dry eye assessment is an important preoperative test before vision correction surgery, as it has a direct impact on postoperative comfort and visual quality.
Many people have varying degrees of dry eye without realizing it, and dryness can temporarily worsen after laser procedures such as LASIK or Femto-LASIK.
Through dry eye tests—such as tear production tests and evaluation of tear film stability—the ophthalmologist can assess the ocular surface and prescribe appropriate treatment before surgery, including lubricating eye drops, artificial tears, or additional therapies if needed.
Treating dry eye before refractive surgery promotes faster healing, reduces burning or stinging sensations, and improves the clarity and stability of vision after the procedure.
For these reasons, dry eye evaluation is considered a core component of the preoperative workup, especially for patients who use contact lenses for long periods or spend extended hours in front of digital screens.
Fundus and Retinal Examination
Fundus and retinal examination is performed to ensure that the internal structures of the eye are healthy before undergoing any laser vision correction procedure.
During this exam, the ophthalmologist dilates the pupil using special eye drops, then carefully examines the retina, optic nerve, and retinal blood vessels to rule out problems such as retinal holes or tears, diabetic retinopathy, or degenerative changes related to high myopia.
If any retinal pathology is detected, preventive treatment may be required before refractive surgery, or certain techniques may be deemed unsuitable to protect the patient’s vision.
A thorough fundus examination also confirms that reduced vision is due solely to refractive errors (such as myopia, hyperopia, or astigmatism), and not to underlying retinal or optic nerve disease.
This evaluation is particularly important for patients with high myopia or a family history of retinal problems, and it is a key step in determining the long-term safety of laser vision correction.

The Most Common Types of Vision Correction Procedures / Latest Vision Correction Techniques
Vision correction procedures have advanced significantly in recent years. Laser-based techniques such as LASIK, Femto-LASIK, and SMILE (Small Incision Lenticule Extraction) are now among the most modern and widely used options for treating myopia (short-sightedness), hyperopia (long-sightedness), and astigmatism.
These procedures work by precisely reshaping the cornea using laser technology to improve the way light is focused onto the retina, thereby reducing or even eliminating the need for prescription glasses or contact lenses.
More advanced options have also emerged, such as surface laser procedures like PRK (Photorefractive Keratectomy) and Custom LASIK, which are tailored to the individual optical characteristics of each eye. In addition, implantable collamer lenses (ICL) are used for patients with high refractive errors or corneas that are not suitable for laser reshaping.
The choice of the most appropriate vision correction procedure depends on several factors, including the health of the eye, corneal thickness, the patient’s age, and lifestyle. For this reason, it is essential to consult a specialized ophthalmologist to determine the safest, most up-to-date, and most suitable technique for each individual case.
LASIK Surgery
LASIK (Laser-Assisted in Situ Keratomileusis) is one of the most common and well‑known procedures for vision correction, used to treat myopia (short-sightedness), hyperopia (long‑sightedness), and astigmatism.
This technique reshapes the corneal surface using an excimer laser after creating a thin flap in the cornea.
LASIK aims to focus light accurately on the retina, allowing most patients to significantly reduce or completely dispense with glasses and contact lenses.
Its main advantages are rapid visual recovery, minimal pain, and improvement in vision within hours to a few days after surgery.
Despite being one of the most widely used modern vision correction techniques, it is not suitable for everyone, particularly patients with thin or irregular corneas.
For this reason, the ophthalmologist selects the most appropriate type of refractive surgery based on a comprehensive eye examination.
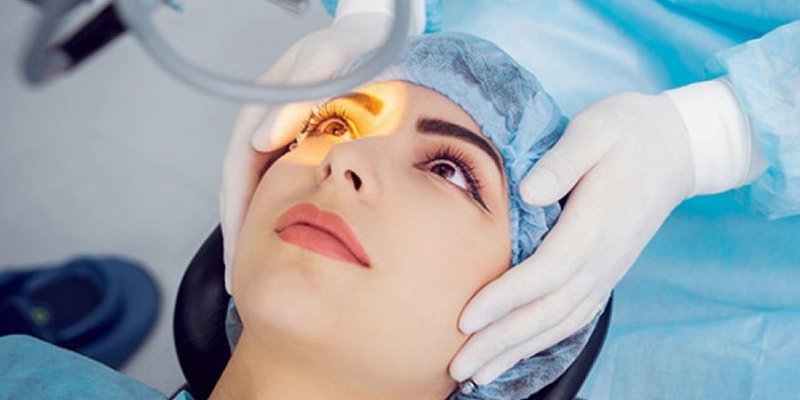
FemtoLASIK
FemtoLASIK represents a more advanced generation of laser vision correction that combines the benefits of conventional LASIK with the precision of femtosecond laser technology.
In this procedure, the corneal flap is created using a femtosecond laser instead of a mechanical microkeratome, which enhances safety and accuracy.
FemtoLASIK effectively treats myopia, hyperopia, and astigmatism (irregular curvature of the cornea) while reducing complications related to flap creation.
It is considered one of the latest refractive surgery options, particularly suitable for patients with relatively thinner or slightly irregular corneas compared to standard LASIK.
It also offers rapid recovery, high‑quality vision, and in many cases a lower incidence of dry eye and night‑vision disturbances such as halos and glare.
The decision to perform FemtoLASIK is made after assessing corneal thickness and the degree of refractive error, as part of a detailed comparison of all available refractive procedures.
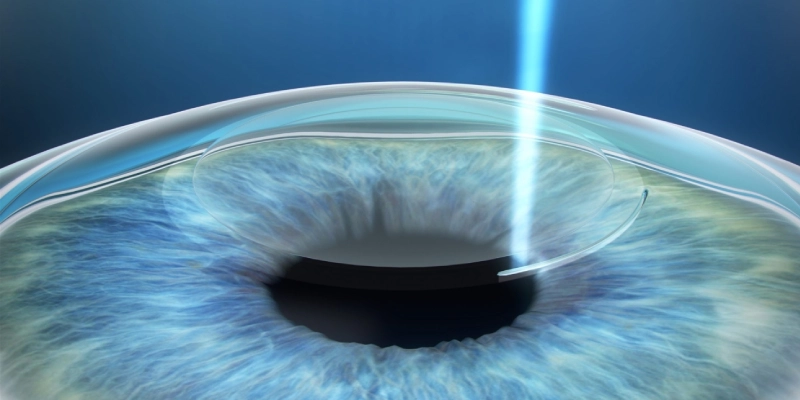
SMILE (Small Incision Lenticule Extraction)
SMILE (Small Incision Lenticule Extraction) is one of the newest laser vision correction techniques, often referred to as “keyhole laser eye surgery.”
In SMILE, no full‑thickness corneal flap is created. Instead, a femtosecond laser is used to sculpt a thin disc of corneal tissue (lenticule) inside the cornea, which is then removed through a very small incision.
This method preserves corneal biomechanics to a greater extent and reduces the risk of postoperative dry eye and corneal weakening.
SMILE is most commonly used to correct myopia and certain degrees of astigmatism and is considered an advanced option for those seeking vision correction with minimal surgical intervention.
It offers fast recovery and a quick return to daily activities, with a gradual stabilization of visual acuity.
SMILE is classified among the latest refractive surgery techniques and is often compared with LASIK and FemtoLASIK to determine the most suitable approach for each case.
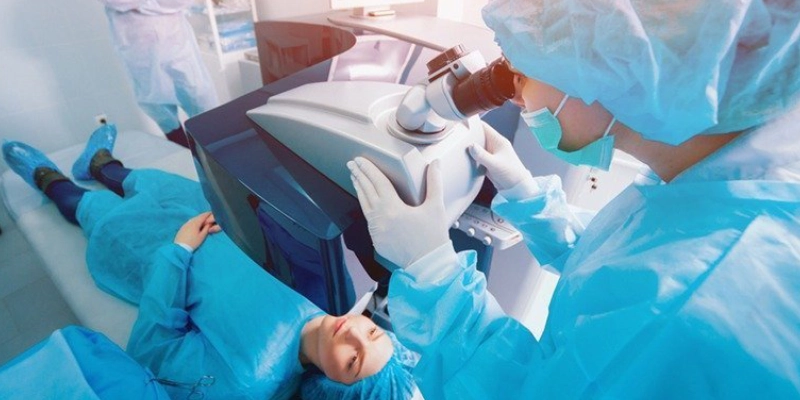
PRK (Photorefractive Keratectomy)
PRK is one of the earliest and most established forms of laser vision correction and is still widely used, especially in patients who are not ideal candidates for LASIK.
In PRK, the thin outer layer of the cornea (the epithelium) is removed, and the underlying corneal surface is reshaped directly with an excimer laser to correct myopia, hyperopia, and astigmatism.
No corneal flap is created in PRK, which makes it a good option for patients with thin corneas or those at higher risk of eye trauma, such as contact sports athletes.
Recovery after PRK is slower than after LASIK, with more discomfort or burning in the first few days; however, the final visual outcomes are generally comparable.
PRK remains a key component of the refractive surgery spectrum, chosen based on corneal thickness, lifestyle, and the degree of refractive error.

Quick Comparison of the Four Main Techniques
The most widely used modern laser vision correction techniques fall into four main categories: LASIK, FemtoLASIK, SMILE, and PRK.
Both LASIK and FemtoLASIK involve creating a corneal flap, with FemtoLASIK offering superior precision and safety through the use of a femtosecond laser instead of a mechanical blade.
SMILE is a more advanced, flap‑less technique that preserves the overall structure and strength of the cornea by using only a small incision, helping to reduce dry eye and corneal complications.
PRK is generally preferred for thin corneas or for patients engaged in high‑impact sports, at the expense of a longer recovery period.
Choosing the “best” procedure does not depend solely on how modern the technique is, but rather on its suitability to corneal status, refractive error, age, and lifestyle.
A detailed consultation with an experienced ophthalmologist remains the most critical step before deciding on any form of refractive surgery.
Vision Correction by Cataract Extraction
Cataract surgery (removal of lens opacity) is a very common procedure that not only treats the cloudy lens but can also significantly improve refractive status.
During the operation, the surgeon removes the opaque natural lens and replaces it with a clear intraocular lens (IOL), usually calculated precisely to correct myopia or hyperopia and, in some cases, astigmatism.
Selecting multifocal IOLs or toric IOLs (for astigmatism) can markedly reduce dependence on glasses after surgery.
Thus, cataract extraction is also considered a form of refractive surgery, especially in older patients who have cataracts in addition to pre‑existing refractive errors.
It is one of the most successful procedures in ophthalmology and can greatly enhance visual function and quality of life, particularly when combined with meticulous preoperative planning of the IOL power and type.
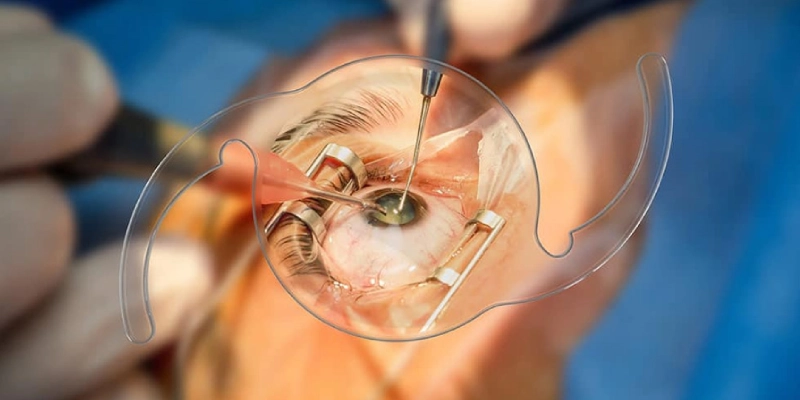
Vision Correction with Intraocular Lens Implantation
Implantable lenses (ICL – Implantable Collamer Lens – or other phakic/additive IOLs) represent an advanced option for patients who are not suitable candidates for corneal laser procedures.
In this technique, a thin, transparent lens is implanted inside the eye, usually in front of the natural lens or in the posterior chamber, without changing the shape of the cornea.
Lens implantation is suitable for high degrees of myopia and hyperopia, and for some patients with thin corneas or early keratoconus, where laser procedures are not recommended.
This method can correct large refractive errors while preserving corneal tissue, with the added advantage that the implanted lens can be removed or replaced if needed.
Intraocular lens implantation is considered one of the most advanced refractive solutions available in specialized eye centers and represents a strategic alternative alongside LASIK, SMILE, and PRK.
Presbyond Technique
Presbyond (laser‑blended vision) is a group of laser techniques specifically developed to address presbyopia (age‑related difficulty with near vision) that typically appears after the age of 40.
Instead of relying on reading glasses, this approach reshapes the cornea of each eye in a customized way to create a “blended” or quasi‑multifocal vision, providing functional vision at near, intermediate, and far distances.
Presbyond is an extension of modern laser vision correction technologies, targeting a large group of people whose options were previously limited once presbyopia developed.
It can be used in patients who have already undergone LASIK, as well as those with mild refractive errors who want to reduce their dependence on reading glasses.
The ophthalmologist determines a patient’s suitability for Presbyond after carefully evaluating lifestyle, occupation, and daily visual demands to achieve the best possible balance between clarity of vision and visual comfort.
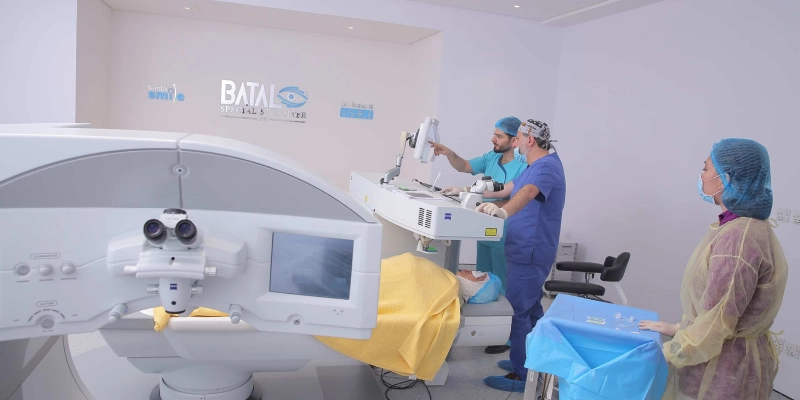
Steps of Vision Correction Surgery
The process of vision correction begins with a visit to an ophthalmologist for a comprehensive eye examination. This includes assessing visual acuity, evaluating the cornea and retina, and measuring intraocular pressure to determine whether the patient is a suitable candidate for laser vision correction procedures such as LASIK, Femto-LASIK, or other advanced techniques.
The doctor then explains the details of the procedure, the expected outcomes, and possible risks, in addition to clarifying the pre‑operative instructions, such as discontinuing contact lens wear for a specified period of time.
On the day of surgery, the eye is numbed with topical anesthetic drops, and an excimer or femtosecond laser is used to accurately reshape the corneal surface in order to correct myopia, hyperopia, or astigmatism. The procedure usually takes about 10–20 minutes for both eyes.
After the surgery, the doctor applies antibiotic and lubricating eye drops and provides detailed post‑operative care instructions, such as avoiding eye rubbing, staying away from dust and bright light, and adhering to follow‑up appointments to ensure visual stability and confirm the success of the operation.
With these integrated steps, vision correction surgery becomes a safe and effective option that can reduce or eliminate dependence on eyeglasses and contact lenses, enhancing both visual quality and overall quality of life.
Pre‑operative preparation
Before undergoing vision correction surgery, the ophthalmologist performs a comprehensive eye examination to assess the severity of the refractive error and determine its type, such as myopia (shortsightedness), hyperopia (longsightedness), or astigmatism.
Pre‑operative assessment typically includes measuring corneal thickness, examining the retina, checking intraocular pressure, and ruling out any ocular diseases that could compromise the outcome of the procedure.
Patients are usually advised to stop wearing contact lenses for a period specified by the doctor before surgery, as lenses can alter the natural shape of the cornea and interfere with the accuracy of the pre‑surgical measurements.
During the consultation, realistic expectations are discussed in detail, along with an explanation of the surgical steps, potential risks, and possible complications, to ensure an informed and well‑considered decision.
This thorough preparation aims to select the most suitable vision correction technique for each individual case—whether LASIK, Femto‑LASIK, or surface ablation techniques such as PRK—and to achieve the best possible visual outcome.
Step‑by‑step surgical procedure
Vision correction surgery begins with topical anesthesia in the form of eye drops to minimize discomfort and help the patient remain relaxed throughout the procedure.
The eye is then stabilized with a special device to prevent movement. The surgeon uses an excimer laser or femtosecond laser to reshape the corneal surface or create a thin corneal flap, depending on the specific technique being used.
In LASIK procedures, a thin flap is created in the cornea and gently lifted. The laser is then applied to the underlying corneal tissue to reshape it and correct the way light is focused onto the retina. Once the laser treatment is complete, the flap is repositioned with high precision.
In surface ablation techniques such as PRK, the very thin outer layer of the cornea (the epithelium) is removed, and the laser is applied directly to the corneal surface. A therapeutic (bandage) contact lens is then placed to protect the eye and support healing.
Throughout the procedure, the patient is asked to focus on a fixation light, while the laser system tracks eye movements and delivers treatment at very high speed and microscopic accuracy, helping to achieve optimal visual acuity.
Procedure duration and pain level
Vision correction surgery is a relatively brief procedure, usually taking around 10–20 minutes for both eyes, while the actual laser application to the cornea lasts only a few seconds to a couple of minutes per eye.
As for pain, most patients experience only minimal discomfort during the surgery, thanks to the use of topical anesthetic drops. The sensation is often described as mild pressure or slight discomfort rather than pain.
After the procedure, patients may experience burning, tearing, or a foreign‑body sensation in the eye for several hours to a few days, depending on the technique used. These symptoms generally improve with the prescribed medicated eye drops and protective measures.
Vision correction surgery is considered a rapid and relatively safe procedure, and most patients notice a significant improvement in their vision quality within the first 24–48 hours, with continued refinement of visual acuity over the following weeks.
Understanding the typical duration of the procedure and the expected level of discomfort helps patients prepare both mentally and physically, and reinforces their confidence in the surgical process and its short‑ and long‑term outcomes.
Recovery Time After Vision Correction Surgery
Recovery after laser vision correction procedures—such as LASIK, Femto-LASIK, and PRK—varies from one person to another, but it generally follows a predictable timeline.
Most patients notice a significant improvement in their vision within 24–48 hours after surgery. Mild dryness or a slight burning sensation in the eyes is common during the first few days.
Visual acuity continues to stabilize over the following weeks, and most people can return to desk work within 2–3 days, provided they avoid prolonged eye strain.
Full recovery and complete stabilization of the final visual outcome typically take between one and three months, depending on the type of procedure and the condition of the cornea before surgery.
Using lubricating eye drops and prescribed medicated drops as directed, avoiding eye rubbing, and staying away from swimming pools, dust, and direct strong sunlight all contribute to faster healing and a lower risk of complications.
It is therefore essential to follow your ophthalmologist’s instructions carefully and attend all scheduled follow-up appointments to ensure stable vision and achieve the best possible results from your vision correction surgery.
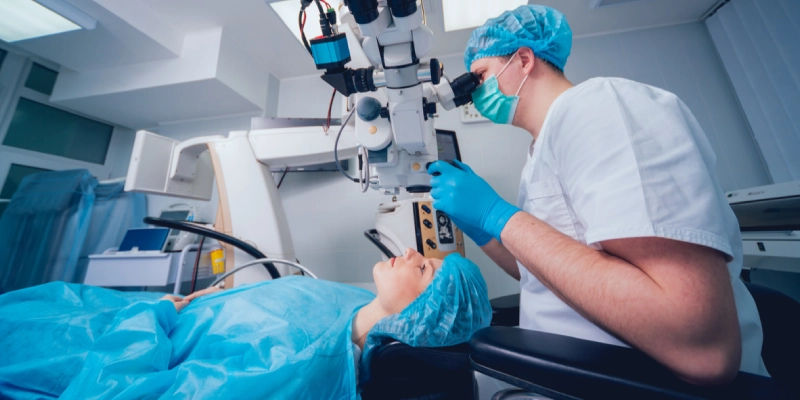
Potential Complications of Vision Correction (and Their Actual Incidence)
Although laser vision correction procedures such as LASIK and SMILE are considered very safe, they are still medical interventions that can be associated with certain complications at varying rates.
Dry eye is the most common side effect after laser vision correction, occurring in about 30–50% of patients during the first few weeks. However, it is usually temporary and responds well to lubricating eye drops.
Blurred or hazy vision and nighttime glare or halos around lights may occur in about 5–10% of patients in the first few months after surgery, and these symptoms usually improve gradually as the cornea heals and vision stabilizes.
Bacterial infection or intraocular inflammation is extremely rare (less than 0.1%), thanks to modern sterilization techniques and strict adherence to postoperative instructions.
Other rare complications, such as corneal biomechanical instability (post-LASIK ectasia or keratoconus-like changes), occur in fewer than 0.05% of cases. Comprehensive preoperative screening significantly reduces the risk of these problems.
The need for an enhancement procedure (retreatment) arises in about 2–5% of patients, particularly in those with high degrees of myopia or hyperopia.
Choosing a specialized center, an experienced refractive surgeon, and carefully following postoperative instructions greatly minimizes these risks and offers the best chance of achieving stable, long-term, and safe visual outcomes.
Cost of Vision Correction Surgery in Jeddah 2026
The cost of vision correction surgery in Jeddah in 2026 varies according to the type of procedure (surface laser PRK, LASIK, Femto-LASIK, SMILE, or phakic IOL implantation), the condition of the eye, and the degree of refractive error, in addition to the reputation of the medical center and the ophthalmic surgeon’s level of experience.
In most cases, prices for vision correction procedures in Jeddah start in the lower thousands per eye, and may increase when using advanced laser platforms or high-precision diagnostic devices for detailed corneal mapping and analysis before surgery.
The total cost of refractive surgery usually covers the preoperative assessment, the surgical procedure itself, and postoperative follow‑up visits. Fees may differ between hospitals and specialized eye centers depending on package deals and whether comprehensive bundles are offered.
When comparing prices for vision correction surgery in Jeddah in 2026, it is important not to base the decision on cost alone, but to consider the quality and technology of the equipment used, the availability of a specialized refractive surgery team, and strict adherence to sterilization and patient safety standards.
Contacting refractive surgery centers in Jeddah directly and undergoing an initial screening helps obtain an accurate cost estimate and compare available options, while ensuring selection of the most medically appropriate solution for safe vision correction and improved eyesight.
Can pregnant women undergo vision correction?
In general, it’s recommended to postpone laser vision correction procedures during pregnancy and breastfeeding. Hormonal changes at these stages can affect corneal thickness and visual acuity, which may lead to inaccurate measurements of refractive errors such as myopia, hyperopia, or astigmatism.
In addition, some medications used before and after vision correction surgery—such as antibiotic eye drops, corticosteroid drops, and mydriatic (pupil‑dilating) drops—may not be completely safe for the fetus or breastfeeding infant.
For this reason, ophthalmologists usually advise against having LASIK, femto-LASIK, or any other form of laser refractive surgery during pregnancy, and recommend postponing it until after delivery and the end of the breastfeeding period, when hormone levels stabilize and vision measurements return to their baseline.
However, if a pregnant woman experiences sudden or significant deterioration in vision, she should see an ophthalmologist immediately to assess the condition and determine the safest treatment approach without putting the pregnancy at risk.
Vision Correction After 40: Is It Right for Everyone?
After the age of forty, age‑related vision problems begin to appear, most notably presbyopia (difficulty focusing on near objects). At this point, many people start looking into vision correction options such as LASIK, SMILE (femto‑SMILE), or intraocular lenses.
Whether vision correction after forty is suitable depends on several key medical factors, including: the degree of refractive error, corneal thickness, the health of the natural lens, early signs of cataract, as well as chronic conditions such as diabetes and hypertension.
Laser vision correction is not appropriate for everyone over forty. In some cases, implanting intraocular lenses or replacing the eye’s natural lens is actually the safest and most effective option to improve both distance and near vision.
For this reason, decisions should not be based on personal anecdotes or advertisements. A comprehensive eye examination by an ophthalmologist is essential, including evaluation of the cornea, crystalline lens, and retina before choosing any vision correction procedure.
Selecting the right technique at this stage of life helps achieve stable vision, reduce dependence on glasses, and maintain long‑term eye health.
Why Batal Eye Specialist Center Is Considered the Leading Vision Correction Center in Jeddah
Batal Eye Specialist Center is recognized as one of the top destinations for vision correction in Jeddah, thanks to its use of state-of-the-art laser technologies, including LASIK, PRK, and SMILE, while adhering to the highest international safety standards and medical protocols.
The center is staffed by a distinguished team of consultant ophthalmologists with extensive experience in refractive surgery and the management of vision disorders such as myopia, hyperopia, and astigmatism. This expertise ensures accurate diagnosis and a fully customized treatment plan tailored to each patient’s visual needs.
Batal Eye Specialist Center is equipped with advanced diagnostic devices for detailed corneal assessment, including corneal thickness measurement and corneal topography mapping. These evaluations are crucial to determining a patient’s suitability for refractive procedures and minimizing the risk of complications.
The center is committed to providing a comprehensive patient experience that starts with the initial consultation, where all available vision correction options are explained clearly and in accessible language. This is followed by meticulous surgical execution and structured postoperative follow-up.
This dedication to quality, safety, and predictable outcomes has made Batal Eye Specialist Center a preferred choice in Jeddah for individuals seeking safe, effective vision correction and a meaningful improvement in both visual clarity and overall quality of life.

Frequently Asked Questions About Vision Correction
Can my vision prescription change after laser eye surgery?
In most cases, results remain stable for years, but natural age-related changes may still occur.
Can both eyes be treated on the same day?
Yes. Modern laser platforms allow safe same-day treatment for both eyes.
How soon can I drive after LASIK?
Most patients can drive within 24–48 hours, depending on clarity and the doctor’s evaluation.
When can I return to the gym or exercise?
Light workouts can resume after a few days; contact sports and swimming require 2–4 weeks.
Is laser eye surgery painful?
No. Numbing drops prevent pain, and most patients feel only mild pressure or temporary dryness.
Can I use my phone or computer after the procedure?
Yes, but only for short periods during the first day to avoid dryness and strain.
What if my corneas are too thin for LASIK?
Alternatives like PRK or ICL lens implantation may be recommended instead.





