Med info
Are You Eligible for Vision Correction Surgery? Key Requirements, Tests and Candidacy Criteria
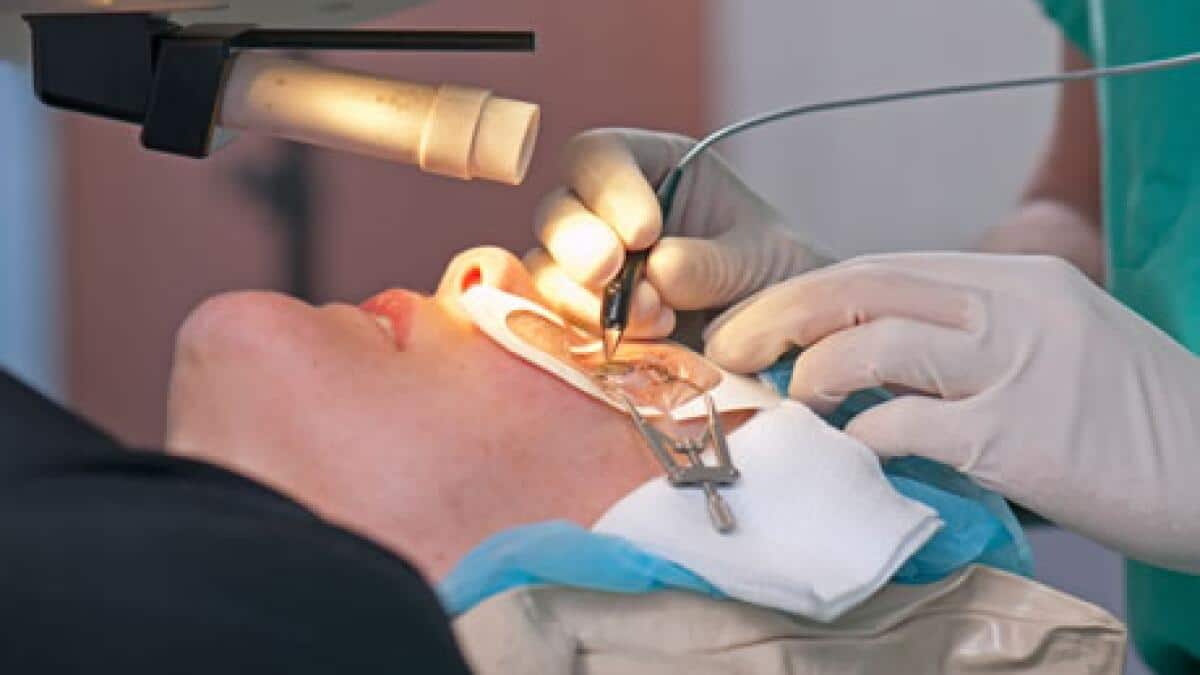
Basic Requirements for Undergoing Vision Correction Surgery
Undergoing vision correction procedures such as LASIK or other laser-based techniques requires meeting several key criteria to ensure safety and achieve reliable results. Generally, the patient should be over 18 years of age, with a stable prescription for at least one to two years, meaning no significant change in eyeglass or contact lens power during that period.
The cornea must be healthy in both thickness and shape, with no evidence of keratoconus, scarring, or chronic inflammation. The patient should also be free from active eye diseases such as severe dry eye, glaucoma, or advanced retinal disorders.
It is also preferable that the patient does not suffer from uncontrolled systemic diseases such as advanced diabetes or autoimmune disorders, as these can interfere with proper corneal healing after laser or LASIK procedures. In addition, certain vision correction techniques are not recommended during pregnancy or breastfeeding.
The basic requirements further include a comprehensive eye examination that covers corneal thickness measurement (pachymetry), retinal evaluation, intraocular pressure measurement, and precise assessment of refractive error, to determine the most appropriate type of vision correction procedure for the patient. Meeting these criteria helps maximize the success rate of vision correction surgery and reduce the risk of complications.

Appropriate Age for Laser Vision Correction
Age is one of the most important basic criteria for undergoing laser vision correction. Ophthalmologists usually recommend that patients be at least 18–21 years old to ensure that the eye has fully developed and the prescription is relatively stable.
Having the procedure at an appropriate age reduces the likelihood of regression (vision worsening again) and improves the long‑term stability of the results.
During the preoperative assessment, the refractive surgeon carefully reviews the patient’s glasses or contact lens prescriptions over previous years to verify that age‑related changes remain within medically acceptable limits.
Stable Prescription for at Least One Year
A stable refractive error for at least one full year is an essential requirement before proceeding with any laser vision correction, such as LASIK or femto‑LASIK.
If the prescription is still changing significantly, laser correction is unlikely to deliver the desired outcome, and the patient may end up needing glasses again or a further corrective procedure.
For this reason, the ophthalmologist asks for documented measurements of myopia, hyperopia, or astigmatism over the last 12 months to confirm stability before considering the patient a suitable candidate for surgery.

Healthy Ocular Tissues and Absence of Infection
For laser vision correction to be successful, the tissues of the eye must be healthy and free of infections or inflammation, such as conjunctivitis, keratitis, or blepharitis.
Active eye inflammation increases the risk of postoperative complications and can interfere with corneal healing and the final visual outcome.
Therefore, the ophthalmologist performs a detailed eye examination to ensure there is no redness, discharge, or severe allergic reaction, and treats any inflammatory condition before scheduling the operation.
Adequate Corneal Thickness for Laser Treatment
Corneal thickness is a critical factor in assessing a patient’s eligibility for laser vision correction, since laser techniques work by reshaping the cornea through removal of precise amounts of corneal tissue.
If the cornea is too thin, performing LASIK may structurally weaken it and raise the risk of complications such as keratoconus‑like ectasia or visual distortions.
To prevent this, a specialized test known as corneal pachymetry or Pentacam tomography is performed to confirm that the cornea is sufficiently thick and meets established safety standards for laser vision correction.
Refraction Assessment and Determining Treatable Range
Refraction testing is a fundamental step in determining candidacy for laser vision correction. Through this exam, the doctor measures the degree of myopia, hyperopia, and astigmatism, and evaluates how far each can be corrected safely with the laser.
Very high refractive errors may not be fully amenable to surface or corneal laser techniques and may be better managed with alternatives such as phakic intraocular lens (IOL) implantation.
Refraction is performed carefully using advanced diagnostic devices in combination with manual subjective refraction to ensure accuracy, helping the surgeon select the most appropriate type of corrective procedure for each patient.
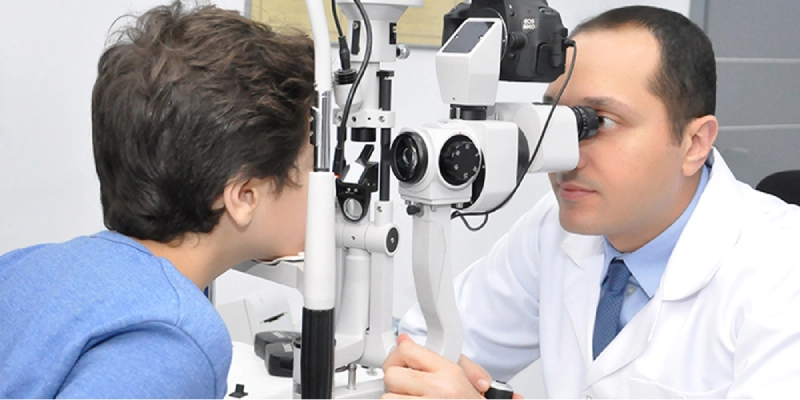
Dilated Fundus Examination to Ensure Retinal Health
A dilated fundus examination is an important prerequisite before deciding on laser vision correction, particularly in patients with high myopia.
This exam allows the doctor to assess the retina and optic nerve, and to detect any retinal holes, tears, or degenerative lesions that may need prophylactic retinal laser treatment prior to corneal refractive surgery.
A healthy retina confirms that the visual problem is primarily refractive rather than due to intraocular disease, thereby improving the likelihood of achieving clear and stable vision after the procedure.
Absence of Systemic Diseases that Impair Corneal Healing
Another key requirement is that the patient be free from uncontrolled systemic conditions known to impair wound healing, such as poorly controlled diabetes mellitus, autoimmune diseases, and certain rheumatologic disorders.
These conditions can slow corneal healing after laser treatment or increase the risk of infection and complications that may compromise visual acuity.
For this reason, the surgeon reviews the patient’s complete medical history and may request additional tests or reports from an internist to ensure that the systemic condition is stable before proceeding with laser vision correction.
Patient’s Ability to Comply with Pre‑ and Postoperative Instructions
The success of laser vision correction depends not only on the surgeon’s expertise and the quality of the technology used, but also on the patient’s adherence to pre‑ and postoperative care instructions.
This includes using prescribed eye drops as directed, avoiding eye rubbing, refraining from eye makeup for a specified period, and attending all scheduled follow‑up appointments.
A patient’s ability and willingness to follow these instructions is considered a fundamental condition for achieving the best possible outcome and minimizing the risk of complications or infection after surgery.
Eligibility Criteria for Vision Correction Procedures by Technique
The requirements for undergoing vision correction surgery vary according to the technique used—such as LASIK, Femto-LASIK, PRK (photorefractive keratectomy), or phakic intraocular lens implantation. Despite these differences, all methods share the need for strict medical criteria to ensure safety and long-term visual stability.
For most refractive procedures, candidates should generally be over 18–21 years of age, with a stable prescription for at least one year. The patient must not have corneal diseases such as keratoconus or significant corneal thinning.
Adequate corneal thickness is essential for LASIK and Femto-LASIK. In cases of thin corneas or very high degrees of myopia or hyperopia, surface laser techniques like PRK or implantable lenses may be more appropriate.
The preoperative assessment includes checking visual acuity, measuring refractive error and astigmatism, performing a fundus examination, and measuring intraocular pressure to rule out glaucoma and retinal disease.
Selecting the optimal vision correction technique depends on detailed examination findings, corneal health, and the patient’s lifestyle. The final decision is made by a refractive surgery specialist to achieve the best possible outcome and minimize the risk of complications.
Criteria for Conventional LASIK
Conventional LASIK is one of the most widely used procedures for vision correction, and it has specific eligibility criteria to ensure safety and successful outcomes.
One of the key requirements is that the patient’s age is usually over 18, with a stable prescription (no significant change in refractive error) for at least one year.
The cornea must be sufficiently thick to allow safe removal of a thin layer during the procedure, and it should be free from conditions such as keratoconus or deep corneal scars.
The patient should not suffer from severe dry eye or active eye infections, and should not have uncontrolled systemic diseases such as poorly controlled diabetes or autoimmune disorders that could interfere with corneal healing.
Adhering to these criteria helps achieve optimal results with conventional LASIK and reduces the risk of complications.
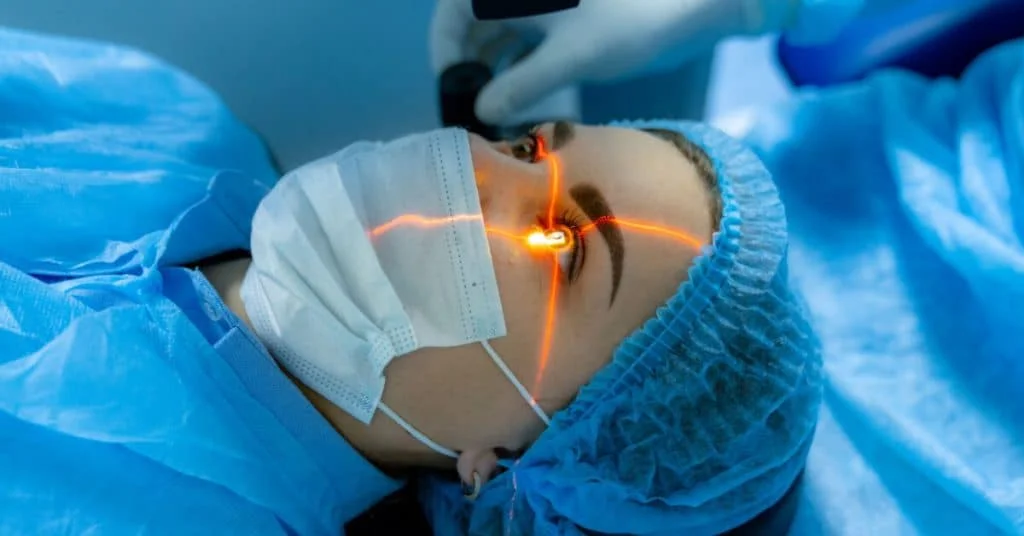
Criteria for Femto-LASIK (Femtosecond LASIK)
Femto-LASIK is an advanced form of LASIK in which a femtosecond laser is used to create the corneal flap instead of a mechanical microkeratome.
Despite the difference in technique, the eligibility criteria for Femto-LASIK largely overlap with those of conventional LASIK: a stable prescription, age typically above 18–21 years, and a healthy, disease-free cornea.
One advantage of Femto-LASIK is that it may be suitable for some patients whose corneal thickness is slightly below what is required for conventional LASIK, while still maintaining a safe minimum residual corneal thickness.
From a medical standpoint, it is often required that the patient is not pregnant or breastfeeding in certain cases, and is not taking medications that could impair tissue healing, with confirmation that there is no severe dry eye or significant ocular allergy.
The decision to perform Femto-LASIK is based on a thorough assessment of the corneal surface and detailed corneal topography to determine whether this technique can correct vision safely.
Criteria for Surface Ablation (PRK)
Photorefractive keratectomy (PRK) is a surface laser procedure used as an alternative for patients who are not ideal candidates for LASIK or Femto-LASIK.
Key criteria for PRK include having myopia, hyperopia, and astigmatism within the treatable range for this technique, with a stable refractive error for at least one year.
PRK is often preferred in patients with relatively thin corneas or those who participate in contact sports or have occupations with a higher risk of ocular trauma, as this procedure does not involve creating a corneal flap.
The cornea must be free from serious structural diseases, and there should be no active eye inflammation or severe dry eye.
The patient should also be aware that the recovery period after PRK is relatively longer than with LASIK, and must be committed to following postoperative instructions and using eye drops for an adequate duration to ensure proper epithelial healing and optimal visual outcomes.
Criteria for Implantable Collamer Lenses (ICL)
Implantable Collamer Lenses (ICL) are an important option for vision correction, especially for high degrees of myopia or in patients who are not suitable candidates for LASIK or surface laser procedures.
One of the main criteria for ICL is that the degree of myopia, hyperopia, or astigmatism falls within the range that ICL lenses are designed to correct, with relatively stable refraction.
The cornea should be healthy, but unlike LASIK, a large corneal thickness is not required, making ICL particularly suitable for patients with thin or laser‑unsuitable corneas.
Other crucial requirements include adequate anterior chamber depth and a sufficient density of corneal endothelial cells to minimize the risk of long-term corneal decompensation.
The patient should not have uncontrolled glaucoma (elevated intraocular pressure) or advanced retinal disease, and a detailed dilated fundus examination is essential before surgery.
Compliance with these criteria ensures that ICL implantation is a safe and effective option among the various methods available for vision correction.
Factors that may limit or affect your eligibility for refractive surgery
Several ocular and general health factors can limit or impact your suitability for vision correction surgery, and all must be carefully evaluated before making a final decision.
One of the most important considerations is the stability of your refractive error over the previous year; for laser vision correction to be successful, your prescription should be relatively stable and not show significant changes.
Corneal thickness and overall corneal health are also fundamental prerequisites. A thin cornea, or the presence of corneal diseases such as keratoconus, can significantly increase the risk of complications and may make the procedure inappropriate.
Uncontrolled chronic conditions—such as poorly managed diabetes or autoimmune diseases—can interfere with proper corneal healing after surgery.
Severe dry eye, recurrent eye infections, or markedly enlarged pupils in dim light are additional factors that can negatively affect the quality of vision after laser refractive surgery.
Pregnancy and breastfeeding, as well as the use of medications that influence hormones or the immune system, may also lead your surgeon to postpone the procedure until your condition has stabilized.
For all these reasons, a comprehensive eye examination, detailed medical history, and advanced corneal imaging are essential steps to determine whether you are a suitable candidate and to accurately assess the safety profile before proceeding with laser vision correction.

Irregular or Thin Cornea
An irregular or abnormally thin cornea is one of the most important factors that can prevent you from being a suitable candidate for laser vision correction.
In such cases, removing corneal tissue during the procedure may significantly weaken the cornea and increase the risk of complications such as keratoconus or progressive loss of visual acuity over time.
For this reason, before approving laser vision correction, the ophthalmologist will perform detailed tests to measure corneal thickness and assess the corneal topography to ensure its stability and structural integrity.
If the cornea is found to be too thin or markedly irregular, the doctor may advise postponing the procedure, choosing alternative refractive techniques, or continuing with glasses or contact lenses to preserve long‑term ocular safety.
Chronic Dry Eye
Chronic dry eye is one of the most common conditions that can affect the outcome of laser vision correction and may even make a patient unsuitable for surgery in some cases.
Laser treatment on the corneal surface can temporarily worsen dry eye symptoms such as burning, stinging, blurred vision, and light sensitivity, which in turn affects visual comfort and overall quality of vision after the procedure.
Before deciding on surgery, the ophthalmologist will evaluate the ocular surface and tear film, and may prescribe lubricating eye drops or specific therapies to manage dry eye and achieve acceptable stability.
If dryness is severe or poorly controlled, the doctor may defer the procedure or advise against it altogether, in order to protect corneal health and secure the best possible refractive outcome.
Pregnancy, Breastfeeding, and Hormonal Changes
Pregnancy and breastfeeding are accompanied by substantial hormonal changes that can affect the stability of your refraction (degree of myopia or hyperopia), making the predicted results of laser vision correction less accurate.
During these phases, corneal thickness, body fluid distribution, and the eye’s need for lubrication may all change, leading to fluctuations in the measurements used to plan the surgery.
Therefore, refractive surgery is usually not recommended during pregnancy or breastfeeding; it is preferable to wait until hormone levels return to baseline and refraction remains stable for a sufficient period.
This waiting period improves the accuracy of the correction planned, and reduces the likelihood of needing an enhancement procedure or additional glasses after recovery.
Use of Medications That Affect Vision Stability
Certain medications can influence the stability of your refraction or corneal healing after refractive surgery, such as hormonal therapies, some antidepressants, isotretinoin‑containing dermatologic drugs, or medications used for chronic diseases.
These drugs may alter the ocular surface, tear production, or intraocular pressure, which can make measurements of your vision unreliable and compromise the safety and effectiveness of laser correction.
Before undergoing any refractive procedure, it is essential to inform your ophthalmologist about all medications and supplements you are taking, so they can assess their potential impact on your eyes and on the treatment plan.
In some cases, the doctor may recommend postponing surgery until a particular medication is discontinued or replaced, or may consider continued use of glasses or contact lenses as the safest option for your eye health.
Family History of Keratoconus
A family history of keratoconus is a major factor that can strongly affect your eligibility for laser vision correction.
Keratoconus is characterized by progressive thinning and weakening of the cornea with a cone‑like protrusion, and it often has a genetic component that increases the risk among family members, especially when the cornea is exposed to surgical alteration.
If keratoconus is present in a parent or sibling, the ophthalmologist will usually perform advanced testing—such as detailed corneal topography and tomography—to detect any early or subclinical signs of the disease.
If these tests reveal a predisposition to keratoconus or early disease, laser vision correction may be strictly contraindicated, and safer alternatives are considered, such as corneal collagen cross‑linking or specialized contact lenses to correct vision without further weakening the cornea.
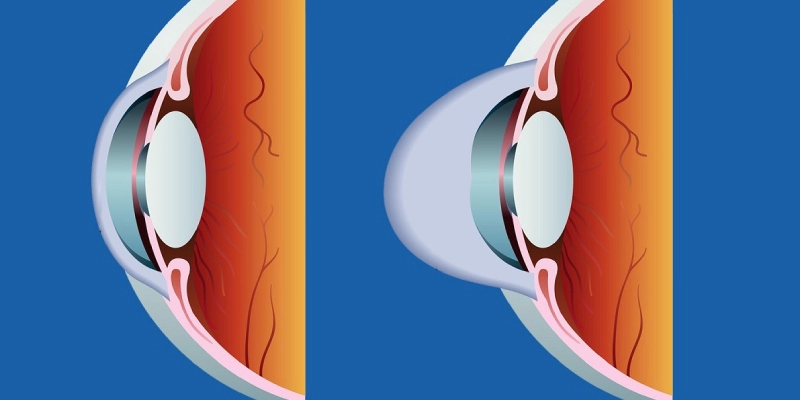
Required Diagnostic Tests Before Determining Eligibility
Before approving any vision correction procedure, your ophthalmologist must perform a series of precise diagnostic tests to confirm that you are a suitable candidate and that your eyes are healthy.
These tests include measuring visual acuity and accurately determining the degree of myopia (short-sightedness), hyperopia (long-sightedness), and astigmatism using advanced diagnostic devices.
A comprehensive corneal assessment is also performed, including corneal thickness measurement (pachymetry) and corneal topography imaging to detect any weakness, thinning, or keratoconus that might make laser vision correction unsafe.
In addition, intraocular pressure is measured to rule out glaucoma, and a detailed examination of the fundus and retina is carried out to ensure there are no tears or retinal diseases that could be adversely affected by the procedure.
These diagnostic evaluations are not merely routine; they are essential for selecting the most appropriate type of refractive surgery, minimizing the risk of complications, and achieving the best possible long-term visual outcomes.
Corneal Topography
Corneal topography is one of the most important diagnostic tests performed before determining a patient’s eligibility for laser vision correction.
This test creates a highly detailed map of the corneal surface to assess its regularity and detect any irregularities or abnormalities, such as early keratoconus.
It helps the ophthalmologist evaluate the safety of procedures like LASIK or Femto‑SMILE and choose the most appropriate type of refractive surgery for each individual case.
Corneal topography is also a key tool for detecting subtle problems that may not appear in a routine eye exam, thereby helping to reduce the risk of complications after vision correction surgery.
Corneal Pachymetry
Corneal pachymetry is an essential component of the preoperative workup before refractive surgery.
This test measures corneal thickness in microns with high precision, which is critical for determining how much corneal tissue can be safely removed during laser treatment.
If the cornea is thinner than the recommended threshold, the patient may be advised to avoid certain procedures, such as conventional LASIK, and opt instead for safer alternatives.
By accurately assessing corneal thickness, pachymetry helps lower the risk of excessive thinning or postoperative ectasia, supporting stable vision and long‑lasting results.
Intraocular Pressure Measurement (IOP)
Measuring intraocular pressure (IOP) is an important step before deciding on laser vision correction.
This test assists in the early detection of elevated eye pressure or a predisposition to glaucoma, both of which require careful evaluation before any corneal surgery.
Abnormal intraocular pressure can affect surgical outcomes and may necessitate modifying the treatment plan or postponing surgery until the condition is controlled.
Including IOP measurement in the preoperative assessment helps protect long‑term eye health and reduces the likelihood of unexpected complications after refractive surgery.
Dry Eye Evaluation
Evaluating dry eye status is a fundamental step before considering any type of vision correction procedure.
Many patients have varying degrees of dry eye without realizing it, and this condition may worsen after LASIK or Femto‑SMILE if not treated in advance.
The ophthalmologist assesses tear quantity, quality, and tear film stability over the corneal surface to determine whether the eyes are ready for surgery or require preliminary treatment.
Managing dry eye before refractive surgery improves visual clarity, reduces postoperative burning and irritation, and speeds up the healing process.
Detailed Refraction Test
A detailed refraction test is the primary examination used to determine the degree of myopia, hyperopia, or astigmatism before vision correction surgery.
Its purpose is to identify the exact lens power that provides the patient with the clearest possible vision, using automated devices and/or subjective refraction with different trial lenses in front of the eyes.
The refraction results form the basis for planning the precise amount of laser correction and for confirming that the prescription is stable before proceeding with surgery.
The more accurate the refraction, the higher the likelihood of achieving optimal outcomes, minimizing the need for enhancement procedures or continued dependence on glasses after surgery.
Who is the ideal candidate for vision correction surgery?
The ideal candidate for vision correction surgery is someone with stable refractive errors—such as myopia (nearsightedness), hyperopia (farsightedness), or astigmatism—for at least one year, and who is typically over 18 years of age with fully developed eyes.
The patient should be in good general health and free from active eye diseases or conditions that could compromise the outcome of surgery, such as keratoconus, severe dry eye, or advanced cataract.
It is also essential that corneal thickness is adequate for the specific laser or surgical technique planned, and that the patient has realistic expectations regarding the results.
Candidacy is confirmed only after a comprehensive eye examination that includes visual acuity testing, corneal thickness (pachymetry) measurement, and refraction assessment, to ensure all safety criteria for vision correction surgery are met and the highest likelihood of success is achieved.
When Are You Not a Good Candidate for Vision Correction Surgery?
Vision correction procedures are generally safe and effective for many people, but they are not suitable for everyone. Certain ocular and general health conditions must be met before undergoing any laser vision correction technique such as LASIK, PRK, or SMILE.
If you have a thin cornea, keratoconus (cone-shaped cornea), or if your prescription (whether myopia, hyperopia, or astigmatism) has not been stable over the past two years, you may not be an ideal candidate for the procedure.
Patients with poorly controlled diabetes, glaucoma, chronic eye inflammation, or severe dry eye that does not respond to treatment are also commonly excluded from these surgeries.
In addition, vision correction procedures are usually postponed for pregnant and breastfeeding women due to hormonal changes that can temporarily alter vision and affect the accuracy and stability of surgical outcomes.
Age is another important factor. These procedures are generally not performed on individuals under 18 years old to ensure that their refractive error has stabilized.
For all these reasons, a comprehensive evaluation by a qualified ophthalmologist remains essential to determine whether you are suitable for vision correction surgery and to choose the most appropriate technique for your specific condition.
Book Now to Check Your Eligibility for Vision Correction Surgery at Batal Specialized Eye Center
Schedule your appointment now at Batal Specialized Eye Center for a comprehensive eye assessment and to determine your suitability for laser or LASIK vision correction, in line with the latest international medical standards.
In a single visit, we perform a full evaluation that includes checking visual acuity, measuring corneal thickness, assessing the stability of your refractive error (eyeglass prescription), and examining the retina to ensure there are no conditions that could make the procedure unsafe.
Our specialized medical team will walk you through all the eligibility criteria for vision correction procedures—such as appropriate age, stable prescription, and absence of active eye diseases—while explaining which type of procedure is most suitable for your eyes.
Booking a consultation at Batal Specialized Eye Center is your first step toward making a safe, well‑informed decision to say goodbye to glasses and contact lenses with confidence and peace of mind.

Frequently Asked Questions About Vision Correction Surgery Eligibility
Q: What are the basic eligibility requirements for vision correction surgery?
Basic requirements include being at least 18–21 years old, having a stable prescription for at least one year, a healthy cornea with adequate thickness, and no active eye diseases such as severe dry eye, glaucoma or advanced retinal disorders. Good general health and realistic expectations are also essential before undergoing any vision correction procedure.
Q: How do I know if my prescription is stable enough for LASIK or other laser procedures?
Your prescription is considered stable when there is no significant change in your eyeglass or contact lens power over at least 12 months. Your ophthalmologist will review previous prescriptions and perform a detailed refraction test to confirm stability before recommending LASIK, PRK or other vision correction options.
Q: Can I have vision correction surgery if I have a thin or irregular cornea?
Patients with thin or irregular corneas may not be suitable candidates for conventional LASIK, as removing corneal tissue could increase the risk of complications such as ectasia. In these cases, your surgeon may recommend alternative options such as PRK, implantable collamer lenses (ICL) or continuing with glasses and contact lenses to protect your long-term eye health.
Q: Who is not a good candidate for vision correction surgery?
You may not be a good candidate if you have keratoconus, very thin corneas, unstable refractive error, uncontrolled diabetes, glaucoma, severe dry eye, chronic eye inflammation, or if you are pregnant or breastfeeding. A comprehensive eye examination is required to identify any contraindications before surgery.
Q: What eye tests are required before vision correction surgery?
Preoperative testing typically includes visual acuity measurement, detailed refraction, corneal topography, corneal pachymetry (thickness measurement), intraocular pressure (IOP) testing, dry eye evaluation and a dilated fundus examination to check the retina and optic nerve. These tests help your surgeon choose the safest and most effective procedure for your eyes.
Q: Does dry eye disease affect my eligibility for LASIK or other laser procedures?
Yes. Chronic or severe dry eye can worsen after LASIK or other laser procedures and may affect visual comfort and clarity. Your ophthalmologist will evaluate your tear film and may recommend treating dry eye first. In some cases of severe dryness, laser vision correction may be postponed or not recommended to protect the cornea.
Q: What is the ideal age range for vision correction surgery?
Most patients are considered for vision correction surgery after the age of 18, once the eyes have finished developing and the prescription has stabilized. Many candidates fall between their early 20s and 40s, but eligibility always depends on individual examination findings, not age alone.
Q: Why should I have my eligibility assessed at Batal Specialized Eye Center?
At Batal Specialized Eye Center, your eligibility is evaluated using advanced diagnostic technology and evidence-based criteria. Our team performs a comprehensive assessment of corneal health, retinal status and refractive stability, and then recommends the safest and most suitable procedure for your lifestyle and visual needs.





